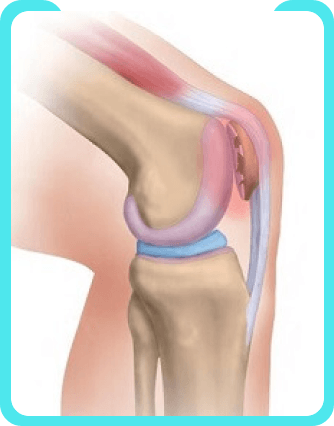

Chondromalacia Patella
- Home
- Conditions
- Knee pain
- Chondromalacia Patella
What is chondromalacia patella?
Chondromalacia Patella, also known as “runner’s knee,” is a condition where the cartilage on the underside of the patella (kneecap) deteriorates and softens. This leads to pain and inflammation in the knee, particularly during activities that put pressure on the knee joint.
Treatment for Chondromalacia Patella
Anatomy of the Knee
The knee joint is one of the most complex joints in the body, consisting of:
Bones: The femur (thigh bone), tibia (shin bone), and patella (kneecap).
Cartilage: Smooth tissue that covers the ends of bones, reducing friction and absorbing shock.
Ligaments: Strong bands of tissue that connect bones and stabilize the knee.
Tendons: Connect muscles to bones, enabling movement.
Synovial Fluid: Lubricates the joint to minimize wear and tear.
Causes of Chondromalacia Patella
Overuse: Repetitive stress from activities like running, jumping, or cycling can wear down the cartilage.
Malalignment: Poor alignment of the kneecap due to congenital factors or muscle imbalances.
Injury: Direct trauma to the knee or previous injuries can damage the cartilage.
Muscle Weakness: Weak thigh muscles can lead to improper tracking of the patella.
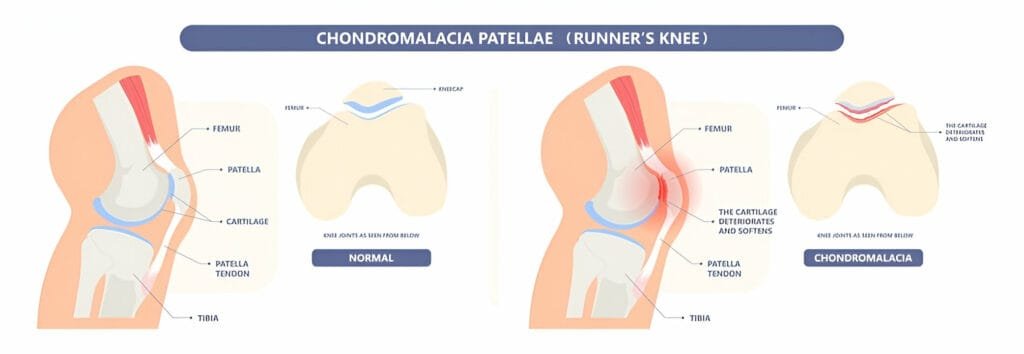

Symptoms of Chondromalacia Patella
Knee Pain: Aching pain in the front of the knee, especially when bending the knee.
Swelling: Mild swelling around the kneecap.
Grinding Sensation: A grinding or crunching feeling when moving the knee.
Stiffness: Difficulty in fully extending or flexing the knee.
Prevention of Chondromalacia Patella
Exercise and Strengthening
Quadriceps Strengthening: Exercises like squats and leg presses to build strong thigh muscles.
Hip Strengthening: Exercises like clamshells and leg lifts to stabilize the pelvis and reduce knee strain.
Core Stability: Strengthening the core muscles to improve overall posture and alignment.
Proper Technique
Proper Footwear: Wear shoes with adequate support and cushioning to reduce knee stress.
Correct Exercise Form: Ensure proper form during physical activities to prevent extreme pressure on the knees.
Weight Management
Maintain a healthy weight to reduce the load on the knee joints and prevent cartilage deterioration.
Regular Stretching
Incorporate regular stretching routines to maintain flexibility and prevent muscle imbalances.
![{"type":"elementor","siteurl":"http:\/\/alleviatepainclinic.com\/wp-json\/","elements":[{"id":"e469b3d","elType":"widget","isInner":false,"isLocked":false,"settings":{"image":{"url":"http:\/\/alleviatepainclinic.com\/wp-content\/uploads\/2024\/05\/Downloader.la-6647086e4615b.jpg","id":18300,"size":"","alt":"","source":"library"},"_margin":{"unit":"px","top":"20","right":"0","bottom":"0","left":"0","isLinked":false},"ha_advanced_tooltip_content":"I am a tooltip","image_size":"large","image_custom_dimension":{"width":"","height":""},"caption_source":"none","caption":"","link_to":"none","link":{"url":"","is_external":"","nofollow":"","custom_attributes":""},"open_lightbox":"default","align":"","align_tablet":"","align_mobile":"","width":{"unit":"%","size":"","sizes":[]},"width_tablet":{"unit":"%","size":"","sizes":[]},"width_mobile":{"unit":"%","size":"","sizes":[]},"space":{"unit":"%","size":"","sizes":[]},"space_tablet":{"unit":"%","size":"","sizes":[]},"space_mobile":{"unit":"%","size":"","sizes":[]},"height":{"unit":"px","size":"","sizes":[]},"height_tablet":{"unit":"px","size":"","sizes":[]},"height_mobile":{"unit":"px","size":"","sizes":[]},"object-fit":"","object-fit_tablet":"","object-fit_mobile":"","object-position":"center center","object-position_tablet":"","object-position_mobile":"","opacity":{"unit":"px","size":"","sizes":[]},"css_filters_css_filter":"","css_filters_blur":{"unit":"px","size":0,"sizes":[]},"css_filters_brightness":{"unit":"px","size":100,"sizes":[]},"css_filters_contrast":{"unit":"px","size":100,"sizes":[]},"css_filters_saturate":{"unit":"px","size":100,"sizes":[]},"css_filters_hue":{"unit":"px","size":0,"sizes":[]},"opacity_hover":{"unit":"px","size":"","sizes":[]},"css_filters_hover_css_filter":"","css_filters_hover_blur":{"unit":"px","size":0,"sizes":[]},"css_filters_hover_brightness":{"unit":"px","size":100,"sizes":[]},"css_filters_hover_contrast":{"unit":"px","size":100,"sizes":[]},"css_filters_hover_saturate":{"unit":"px","size":100,"sizes":[]},"css_filters_hover_hue":{"unit":"px","size":0,"sizes":[]},"background_hover_transition":{"unit":"px","size":"","sizes":[]},"hover_animation":"","image_border_border":"","image_border_width":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"image_border_width_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"image_border_width_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"image_border_color":"","image_border_radius":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"image_border_radius_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"image_border_radius_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"image_box_shadow_box_shadow_type":"","image_box_shadow_box_shadow":{"horizontal":0,"vertical":0,"blur":10,"spread":0,"color":"rgba(0,0,0,0.5)"},"caption_align":"","caption_align_tablet":"","caption_align_mobile":"","text_color":"","caption_background_color":"","caption_typography_typography":"","caption_typography_font_family":"","caption_typography_font_size":{"unit":"px","size":"","sizes":[]},"caption_typography_font_size_tablet":{"unit":"px","size":"","sizes":[]},"caption_typography_font_size_mobile":{"unit":"px","size":"","sizes":[]},"caption_typography_font_weight":"","caption_typography_text_transform":"","caption_typography_font_style":"","caption_typography_text_decoration":"","caption_typography_line_height":{"unit":"px","size":"","sizes":[]},"caption_typography_line_height_tablet":{"unit":"em","size":"","sizes":[]},"caption_typography_line_height_mobile":{"unit":"em","size":"","sizes":[]},"caption_typography_letter_spacing":{"unit":"px","size":"","sizes":[]},"caption_typography_letter_spacing_tablet":{"unit":"px","size":"","sizes":[]},"caption_typography_letter_spacing_mobile":{"unit":"px","size":"","sizes":[]},"caption_typography_word_spacing":{"unit":"px","size":"","sizes":[]},"caption_typography_word_spacing_tablet":{"unit":"em","size":"","sizes":[]},"caption_typography_word_spacing_mobile":{"unit":"em","size":"","sizes":[]},"caption_text_shadow_text_shadow_type":"","caption_text_shadow_text_shadow":{"horizontal":0,"vertical":0,"blur":10,"color":"rgba(0,0,0,0.3)"},"caption_space":{"unit":"px","size":"","sizes":[]},"caption_space_tablet":{"unit":"px","size":"","sizes":[]},"caption_space_mobile":{"unit":"px","size":"","sizes":[]},"_title":"","_margin_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_margin_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_padding":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_padding_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_padding_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_element_width":"","_element_width_tablet":"","_element_width_mobile":"","_element_custom_width":{"unit":"%","size":"","sizes":[]},"_element_custom_width_tablet":{"unit":"px","size":"","sizes":[]},"_element_custom_width_mobile":{"unit":"px","size":"","sizes":[]},"_flex_align_self":"","_flex_align_self_tablet":"","_flex_align_self_mobile":"","_flex_order":"","_flex_order_tablet":"","_flex_order_mobile":"","_flex_order_custom":"","_flex_order_custom_tablet":"","_flex_order_custom_mobile":"","_flex_size":"","_flex_size_tablet":"","_flex_size_mobile":"","_flex_grow":1,"_flex_grow_tablet":"","_flex_grow_mobile":"","_flex_shrink":1,"_flex_shrink_tablet":"","_flex_shrink_mobile":"","_element_vertical_align":"","_element_vertical_align_tablet":"","_element_vertical_align_mobile":"","_position":"","_offset_orientation_h":"start","_offset_x":{"unit":"px","size":0,"sizes":[]},"_offset_x_tablet":{"unit":"px","size":"","sizes":[]},"_offset_x_mobile":{"unit":"px","size":"","sizes":[]},"_offset_x_end":{"unit":"px","size":0,"sizes":[]},"_offset_x_end_tablet":{"unit":"px","size":"","sizes":[]},"_offset_x_end_mobile":{"unit":"px","size":"","sizes":[]},"_offset_orientation_v":"start","_offset_y":{"unit":"px","size":0,"sizes":[]},"_offset_y_tablet":{"unit":"px","size":"","sizes":[]},"_offset_y_mobile":{"unit":"px","size":"","sizes":[]},"_offset_y_end":{"unit":"px","size":0,"sizes":[]},"_offset_y_end_tablet":{"unit":"px","size":"","sizes":[]},"_offset_y_end_mobile":{"unit":"px","size":"","sizes":[]},"_z_index":"","_z_index_tablet":"","_z_index_mobile":"","_element_id":"","_css_classes":"","ha_floating_fx":"","ha_floating_fx_translate_toggle":"","ha_floating_fx_translate_x":{"unit":"px","size":"","sizes":{"from":0,"to":5}},"ha_floating_fx_translate_y":{"unit":"px","size":"","sizes":{"from":0,"to":5}},"ha_floating_fx_translate_duration":{"unit":"px","size":1000,"sizes":[]},"ha_floating_fx_translate_delay":{"unit":"px","size":"","sizes":[]},"ha_floating_fx_rotate_toggle":"","ha_floating_fx_rotate_x":{"unit":"px","size":"","sizes":{"from":0,"to":45}},"ha_floating_fx_rotate_y":{"unit":"px","size":"","sizes":{"from":0,"to":45}},"ha_floating_fx_rotate_z":{"unit":"px","size":"","sizes":{"from":0,"to":45}},"ha_floating_fx_rotate_duration":{"unit":"px","size":1000,"sizes":[]},"ha_floating_fx_rotate_delay":{"unit":"px","size":"","sizes":[]},"ha_floating_fx_scale_toggle":"","ha_floating_fx_scale_x":{"unit":"px","size":"","sizes":{"from":1,"to":1.2}},"ha_floating_fx_scale_y":{"unit":"px","size":"","sizes":{"from":1,"to":1.2}},"ha_floating_fx_scale_duration":{"unit":"px","size":1000,"sizes":[]},"ha_floating_fx_scale_delay":{"unit":"px","size":"","sizes":[]},"ha_element_link":{"url":"","is_external":"","nofollow":"","custom_attributes":""},"ha_transform_fx":"","ha_transform_fx_translate_toggle":"","ha_transform_fx_translate_x":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_x_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_x_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_y":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_y_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_y_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_toggle":"","ha_transform_fx_rotate_mode":"loose","ha_transform_fx_rotate_x":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_x_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_x_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_y":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_y_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_y_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_z":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_z_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_z_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_scale_toggle":"","ha_transform_fx_scale_mode":"loose","ha_transform_fx_scale_x":{"unit":"px","size":1,"sizes":[]},"ha_transform_fx_scale_x_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_scale_x_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_scale_y":{"unit":"px","size":1,"sizes":[]},"ha_transform_fx_scale_y_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_scale_y_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_toggle":"","ha_transform_fx_skew_x":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_x_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_x_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_y":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_y_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_y_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_toggle_hover":"","ha_transform_fx_translate_x_hover":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_x_hover_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_x_hover_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_y_hover":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_y_hover_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_y_hover_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_toggle_hover":"","ha_transform_fx_rotate_mode_hover":"loose","ha_transform_fx_rotate_x_hover":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_x_hover_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_x_hover_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_y_hover":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_y_hover_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_y_hover_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_z_hover":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_z_hover_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_z_hover_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_scale_toggle_hover":"","ha_transform_fx_scale_mode_hover":"loose","ha_transform_fx_scale_x_hover":{"unit":"px","size":1,"sizes":[]},"ha_transform_fx_scale_x_hover_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_scale_x_hover_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_scale_y_hover":{"unit":"px","size":1,"sizes":[]},"ha_transform_fx_scale_y_hover_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_scale_y_hover_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_toggle_hover":"","ha_transform_fx_skew_x_hover":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_x_hover_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_x_hover_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_y_hover":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_y_hover_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_y_hover_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_transition_duration":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_enable":"","ha_advanced_tooltip_position":"top","ha_advanced_tooltip_position_tablet":"","ha_advanced_tooltip_position_mobile":"","ha_advanced_tooltip_animation":"","ha_advanced_tooltip_duration":1000,"ha_advanced_tooltip_arrow":"true","ha_advanced_tooltip_trigger":"hover","ha_advanced_tooltip_distance":{"unit":"px","size":"0","sizes":[]},"ha_advanced_tooltip_distance_tablet":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_distance_mobile":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_align":"center","ha_advanced_tooltip_align_tablet":"","ha_advanced_tooltip_align_mobile":"","ha_advanced_tooltip_width":{"unit":"px","size":"120","sizes":[]},"ha_advanced_tooltip_width_tablet":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_width_mobile":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_arrow_size":{"unit":"px","size":"5","sizes":[]},"ha_advanced_tooltip_arrow_size_tablet":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_arrow_size_mobile":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_typography_typography":"yes","ha_advanced_tooltip_typography_font_family":"Nunito","ha_advanced_tooltip_typography_font_size":{"unit":"px","size":"14","sizes":[]},"ha_advanced_tooltip_typography_font_size_tablet":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_typography_font_size_mobile":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_typography_font_weight":"500","ha_advanced_tooltip_typography_text_transform":"","ha_advanced_tooltip_typography_font_style":"","ha_advanced_tooltip_typography_text_decoration":"","ha_advanced_tooltip_typography_line_height":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_typography_line_height_tablet":{"unit":"em","size":"","sizes":[]},"ha_advanced_tooltip_typography_line_height_mobile":{"unit":"em","size":"","sizes":[]},"ha_advanced_tooltip_typography_letter_spacing":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_typography_letter_spacing_tablet":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_typography_letter_spacing_mobile":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_typography_word_spacing":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_typography_word_spacing_tablet":{"unit":"em","size":"","sizes":[]},"ha_advanced_tooltip_typography_word_spacing_mobile":{"unit":"em","size":"","sizes":[]},"ha_advanced_tooltip_title_section_bg_color_background":"","ha_advanced_tooltip_title_section_bg_color_color":"","ha_advanced_tooltip_title_section_bg_color_color_stop":{"unit":"%","size":0,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_color_stop_tablet":{"unit":"%"},"ha_advanced_tooltip_title_section_bg_color_color_stop_mobile":{"unit":"%"},"ha_advanced_tooltip_title_section_bg_color_color_b":"#f2295b","ha_advanced_tooltip_title_section_bg_color_color_b_stop":{"unit":"%","size":100,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_color_b_stop_tablet":{"unit":"%"},"ha_advanced_tooltip_title_section_bg_color_color_b_stop_mobile":{"unit":"%"},"ha_advanced_tooltip_title_section_bg_color_gradient_type":"linear","ha_advanced_tooltip_title_section_bg_color_gradient_angle":{"unit":"deg","size":180,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_gradient_angle_tablet":{"unit":"deg"},"ha_advanced_tooltip_title_section_bg_color_gradient_angle_mobile":{"unit":"deg"},"ha_advanced_tooltip_title_section_bg_color_gradient_position":"center center","ha_advanced_tooltip_title_section_bg_color_gradient_position_tablet":"","ha_advanced_tooltip_title_section_bg_color_gradient_position_mobile":"","ha_advanced_tooltip_title_section_bg_color_image":{"url":"","id":"","size":""},"ha_advanced_tooltip_title_section_bg_color_image_tablet":{"url":"","id":"","size":""},"ha_advanced_tooltip_title_section_bg_color_image_mobile":{"url":"","id":"","size":""},"ha_advanced_tooltip_title_section_bg_color_position":"","ha_advanced_tooltip_title_section_bg_color_position_tablet":"","ha_advanced_tooltip_title_section_bg_color_position_mobile":"","ha_advanced_tooltip_title_section_bg_color_xpos":{"unit":"px","size":0,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_xpos_tablet":{"unit":"px","size":0,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_xpos_mobile":{"unit":"px","size":0,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_ypos":{"unit":"px","size":0,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_ypos_tablet":{"unit":"px","size":0,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_ypos_mobile":{"unit":"px","size":0,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_attachment":"","ha_advanced_tooltip_title_section_bg_color_repeat":"","ha_advanced_tooltip_title_section_bg_color_repeat_tablet":"","ha_advanced_tooltip_title_section_bg_color_repeat_mobile":"","ha_advanced_tooltip_title_section_bg_color_size":"","ha_advanced_tooltip_title_section_bg_color_size_tablet":"","ha_advanced_tooltip_title_section_bg_color_size_mobile":"","ha_advanced_tooltip_title_section_bg_color_bg_width":{"unit":"%","size":100,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_bg_width_tablet":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_title_section_bg_color_bg_width_mobile":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_title_section_bg_color_video_link":"","ha_advanced_tooltip_title_section_bg_color_video_start":"","ha_advanced_tooltip_title_section_bg_color_video_end":"","ha_advanced_tooltip_title_section_bg_color_play_once":"","ha_advanced_tooltip_title_section_bg_color_play_on_mobile":"","ha_advanced_tooltip_title_section_bg_color_privacy_mode":"","ha_advanced_tooltip_title_section_bg_color_video_fallback":{"url":"","id":"","size":""},"ha_advanced_tooltip_title_section_bg_color_slideshow_gallery":[],"ha_advanced_tooltip_title_section_bg_color_slideshow_loop":"yes","ha_advanced_tooltip_title_section_bg_color_slideshow_slide_duration":5000,"ha_advanced_tooltip_title_section_bg_color_slideshow_slide_transition":"fade","ha_advanced_tooltip_title_section_bg_color_slideshow_transition_duration":500,"ha_advanced_tooltip_title_section_bg_color_slideshow_background_size":"","ha_advanced_tooltip_title_section_bg_color_slideshow_background_size_tablet":"","ha_advanced_tooltip_title_section_bg_color_slideshow_background_size_mobile":"","ha_advanced_tooltip_title_section_bg_color_slideshow_background_position":"","ha_advanced_tooltip_title_section_bg_color_slideshow_background_position_tablet":"","ha_advanced_tooltip_title_section_bg_color_slideshow_background_position_mobile":"","ha_advanced_tooltip_title_section_bg_color_slideshow_lazyload":"","ha_advanced_tooltip_title_section_bg_color_slideshow_ken_burns":"","ha_advanced_tooltip_title_section_bg_color_slideshow_ken_burns_zoom_direction":"in","ha_advanced_tooltip_background_color":"#000000","ha_advanced_tooltip_color":"#ffffff","ha_advanced_tooltip_border_border":"","ha_advanced_tooltip_border_width":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"ha_advanced_tooltip_border_width_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"ha_advanced_tooltip_border_width_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"ha_advanced_tooltip_border_color":"","ha_advanced_tooltip_border_radius":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"ha_advanced_tooltip_border_radius_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"ha_advanced_tooltip_border_radius_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"ha_advanced_tooltip_padding":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"ha_advanced_tooltip_padding_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"ha_advanced_tooltip_padding_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"ha_advanced_tooltip_box_shadow_box_shadow_type":"","ha_advanced_tooltip_box_shadow_box_shadow":{"horizontal":0,"vertical":0,"blur":10,"spread":0,"color":"rgba(0,0,0,0.5)"},"ha_advanced_tooltip_box_shadow_box_shadow_position":" ","jltma_section_element_link":{"url":"","is_external":"","nofollow":"","custom_attributes":""},"_animation":"","_animation_tablet":"","_animation_mobile":"","animation_duration":"","_animation_delay":"","_transform_rotate_popover":"","_transform_rotateZ_effect":{"unit":"px","size":"","sizes":[]},"_transform_rotateZ_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateZ_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_rotate_3d":"","_transform_rotateX_effect":{"unit":"px","size":"","sizes":[]},"_transform_rotateX_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateX_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_rotateY_effect":{"unit":"px","size":"","sizes":[]},"_transform_rotateY_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateY_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_perspective_effect":{"unit":"px","size":"","sizes":[]},"_transform_perspective_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_perspective_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_translate_popover":"","_transform_translateX_effect":{"unit":"px","size":"","sizes":[]},"_transform_translateX_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_translateX_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scale_popover":"","_transform_keep_proportions":"yes","_transform_scale_effect":{"unit":"px","size":"","sizes":[]},"_transform_scale_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scale_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_skew_popover":"","_transform_skewX_effect":{"unit":"px","size":"","sizes":[]},"_transform_skewX_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_skewX_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_skewY_effect":{"unit":"px","size":"","sizes":[]},"_transform_skewY_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_skewY_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_flipX_effect":"","_transform_flipY_effect":"","_transform_rotate_popover_hover":"","_transform_rotateZ_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_rotateZ_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateZ_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_rotate_3d_hover":"","_transform_rotateX_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_rotateX_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateX_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_rotateY_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_rotateY_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateY_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_perspective_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_perspective_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_perspective_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_translate_popover_hover":"","_transform_translateX_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_translateX_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_translateX_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scale_popover_hover":"","_transform_keep_proportions_hover":"yes","_transform_scale_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_scale_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scale_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_skew_popover_hover":"","_transform_skewX_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_skewX_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_skewX_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_skewY_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_skewY_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_skewY_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_flipX_effect_hover":"","_transform_flipY_effect_hover":"","_transform_transition_hover":{"unit":"px","size":"","sizes":[]},"motion_fx_transform_x_anchor_point":"","motion_fx_transform_x_anchor_point_tablet":"","motion_fx_transform_x_anchor_point_mobile":"","motion_fx_transform_y_anchor_point":"","motion_fx_transform_y_anchor_point_tablet":"","motion_fx_transform_y_anchor_point_mobile":"","_background_background":"","_background_color":"","_background_color_stop":{"unit":"%","size":0,"sizes":[]},"_background_color_stop_tablet":{"unit":"%"},"_background_color_stop_mobile":{"unit":"%"},"_background_color_b":"#f2295b","_background_color_b_stop":{"unit":"%","size":100,"sizes":[]},"_background_color_b_stop_tablet":{"unit":"%"},"_background_color_b_stop_mobile":{"unit":"%"},"_background_gradient_type":"linear","_background_gradient_angle":{"unit":"deg","size":180,"sizes":[]},"_background_gradient_angle_tablet":{"unit":"deg"},"_background_gradient_angle_mobile":{"unit":"deg"},"_background_gradient_position":"center center","_background_gradient_position_tablet":"","_background_gradient_position_mobile":"","_background_image":{"url":"","id":"","size":""},"_background_image_tablet":{"url":"","id":"","size":""},"_background_image_mobile":{"url":"","id":"","size":""},"_background_position":"","_background_position_tablet":"","_background_position_mobile":"","_background_xpos":{"unit":"px","size":0,"sizes":[]},"_background_xpos_tablet":{"unit":"px","size":0,"sizes":[]},"_background_xpos_mobile":{"unit":"px","size":0,"sizes":[]},"_background_ypos":{"unit":"px","size":0,"sizes":[]},"_background_ypos_tablet":{"unit":"px","size":0,"sizes":[]},"_background_ypos_mobile":{"unit":"px","size":0,"sizes":[]},"_background_attachment":"","_background_repeat":"","_background_repeat_tablet":"","_background_repeat_mobile":"","_background_size":"","_background_size_tablet":"","_background_size_mobile":"","_background_bg_width":{"unit":"%","size":100,"sizes":[]},"_background_bg_width_tablet":{"unit":"px","size":"","sizes":[]},"_background_bg_width_mobile":{"unit":"px","size":"","sizes":[]},"_background_video_link":"","_background_video_start":"","_background_video_end":"","_background_play_once":"","_background_play_on_mobile":"","_background_privacy_mode":"","_background_video_fallback":{"url":"","id":"","size":""},"_background_slideshow_gallery":[],"_background_slideshow_loop":"yes","_background_slideshow_slide_duration":5000,"_background_slideshow_slide_transition":"fade","_background_slideshow_transition_duration":500,"_background_slideshow_background_size":"","_background_slideshow_background_size_tablet":"","_background_slideshow_background_size_mobile":"","_background_slideshow_background_position":"","_background_slideshow_background_position_tablet":"","_background_slideshow_background_position_mobile":"","_background_slideshow_lazyload":"","_background_slideshow_ken_burns":"","_background_slideshow_ken_burns_zoom_direction":"in","_background_hover_background":"","_background_hover_color":"","_background_hover_color_stop":{"unit":"%","size":0,"sizes":[]},"_background_hover_color_stop_tablet":{"unit":"%"},"_background_hover_color_stop_mobile":{"unit":"%"},"_background_hover_color_b":"#f2295b","_background_hover_color_b_stop":{"unit":"%","size":100,"sizes":[]},"_background_hover_color_b_stop_tablet":{"unit":"%"},"_background_hover_color_b_stop_mobile":{"unit":"%"},"_background_hover_gradient_type":"linear","_background_hover_gradient_angle":{"unit":"deg","size":180,"sizes":[]},"_background_hover_gradient_angle_tablet":{"unit":"deg"},"_background_hover_gradient_angle_mobile":{"unit":"deg"},"_background_hover_gradient_position":"center center","_background_hover_gradient_position_tablet":"","_background_hover_gradient_position_mobile":"","_background_hover_image":{"url":"","id":"","size":""},"_background_hover_image_tablet":{"url":"","id":"","size":""},"_background_hover_image_mobile":{"url":"","id":"","size":""},"_background_hover_position":"","_background_hover_position_tablet":"","_background_hover_position_mobile":"","_background_hover_xpos":{"unit":"px","size":0,"sizes":[]},"_background_hover_xpos_tablet":{"unit":"px","size":0,"sizes":[]},"_background_hover_xpos_mobile":{"unit":"px","size":0,"sizes":[]},"_background_hover_ypos":{"unit":"px","size":0,"sizes":[]},"_background_hover_ypos_tablet":{"unit":"px","size":0,"sizes":[]},"_background_hover_ypos_mobile":{"unit":"px","size":0,"sizes":[]},"_background_hover_attachment":"","_background_hover_repeat":"","_background_hover_repeat_tablet":"","_background_hover_repeat_mobile":"","_background_hover_size":"","_background_hover_size_tablet":"","_background_hover_size_mobile":"","_background_hover_bg_width":{"unit":"%","size":100,"sizes":[]},"_background_hover_bg_width_tablet":{"unit":"px","size":"","sizes":[]},"_background_hover_bg_width_mobile":{"unit":"px","size":"","sizes":[]},"_background_hover_video_link":"","_background_hover_video_start":"","_background_hover_video_end":"","_background_hover_play_once":"","_background_hover_play_on_mobile":"","_background_hover_privacy_mode":"","_background_hover_video_fallback":{"url":"","id":"","size":""},"_background_hover_slideshow_gallery":[],"_background_hover_slideshow_loop":"yes","_background_hover_slideshow_slide_duration":5000,"_background_hover_slideshow_slide_transition":"fade","_background_hover_slideshow_transition_duration":500,"_background_hover_slideshow_background_size":"","_background_hover_slideshow_background_size_tablet":"","_background_hover_slideshow_background_size_mobile":"","_background_hover_slideshow_background_position":"","_background_hover_slideshow_background_position_tablet":"","_background_hover_slideshow_background_position_mobile":"","_background_hover_slideshow_lazyload":"","_background_hover_slideshow_ken_burns":"","_background_hover_slideshow_ken_burns_zoom_direction":"in","_background_hover_transition":{"unit":"px","size":"","sizes":[]},"jltma_enable_glassmorphism_effect":"no","jltma_glass_effect_blur_value":20,"_ha_background_overlay_background":"","_ha_background_overlay_color":"","_ha_background_overlay_color_stop":{"unit":"%","size":0,"sizes":[]},"_ha_background_overlay_color_stop_tablet":{"unit":"%"},"_ha_background_overlay_color_stop_mobile":{"unit":"%"},"_ha_background_overlay_color_b":"#f2295b","_ha_background_overlay_color_b_stop":{"unit":"%","size":100,"sizes":[]},"_ha_background_overlay_color_b_stop_tablet":{"unit":"%"},"_ha_background_overlay_color_b_stop_mobile":{"unit":"%"},"_ha_background_overlay_gradient_type":"linear","_ha_background_overlay_gradient_angle":{"unit":"deg","size":180,"sizes":[]},"_ha_background_overlay_gradient_angle_tablet":{"unit":"deg"},"_ha_background_overlay_gradient_angle_mobile":{"unit":"deg"},"_ha_background_overlay_gradient_position":"center center","_ha_background_overlay_gradient_position_tablet":"","_ha_background_overlay_gradient_position_mobile":"","_ha_background_overlay_image":{"url":"","id":"","size":""},"_ha_background_overlay_image_tablet":{"url":"","id":"","size":""},"_ha_background_overlay_image_mobile":{"url":"","id":"","size":""},"_ha_background_overlay_position":"","_ha_background_overlay_position_tablet":"","_ha_background_overlay_position_mobile":"","_ha_background_overlay_xpos":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_xpos_tablet":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_xpos_mobile":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_ypos":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_ypos_tablet":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_ypos_mobile":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_attachment":"","_ha_background_overlay_repeat":"","_ha_background_overlay_repeat_tablet":"","_ha_background_overlay_repeat_mobile":"","_ha_background_overlay_size":"","_ha_background_overlay_size_tablet":"","_ha_background_overlay_size_mobile":"","_ha_background_overlay_bg_width":{"unit":"%","size":100,"sizes":[]},"_ha_background_overlay_bg_width_tablet":{"unit":"px","size":"","sizes":[]},"_ha_background_overlay_bg_width_mobile":{"unit":"px","size":"","sizes":[]},"_ha_background_overlay_video_link":"","_ha_background_overlay_video_start":"","_ha_background_overlay_video_end":"","_ha_background_overlay_play_once":"","_ha_background_overlay_play_on_mobile":"","_ha_background_overlay_privacy_mode":"","_ha_background_overlay_video_fallback":{"url":"","id":"","size":""},"_ha_background_overlay_slideshow_gallery":[],"_ha_background_overlay_slideshow_loop":"yes","_ha_background_overlay_slideshow_slide_duration":5000,"_ha_background_overlay_slideshow_slide_transition":"fade","_ha_background_overlay_slideshow_transition_duration":500,"_ha_background_overlay_slideshow_background_size":"","_ha_background_overlay_slideshow_background_size_tablet":"","_ha_background_overlay_slideshow_background_size_mobile":"","_ha_background_overlay_slideshow_background_position":"","_ha_background_overlay_slideshow_background_position_tablet":"","_ha_background_overlay_slideshow_background_position_mobile":"","_ha_background_overlay_slideshow_lazyload":"","_ha_background_overlay_slideshow_ken_burns":"","_ha_background_overlay_slideshow_ken_burns_zoom_direction":"in","_ha_background_overlay_opacity":{"unit":"px","size":0.5,"sizes":[]},"_ha_css_filters_css_filter":"","_ha_css_filters_blur":{"unit":"px","size":0,"sizes":[]},"_ha_css_filters_brightness":{"unit":"px","size":100,"sizes":[]},"_ha_css_filters_contrast":{"unit":"px","size":100,"sizes":[]},"_ha_css_filters_saturate":{"unit":"px","size":100,"sizes":[]},"_ha_css_filters_hue":{"unit":"px","size":0,"sizes":[]},"_ha_overlay_blend_mode":"","_ha_background_overlay_hover_background":"","_ha_background_overlay_hover_color":"","_ha_background_overlay_hover_color_stop":{"unit":"%","size":0,"sizes":[]},"_ha_background_overlay_hover_color_stop_tablet":{"unit":"%"},"_ha_background_overlay_hover_color_stop_mobile":{"unit":"%"},"_ha_background_overlay_hover_color_b":"#f2295b","_ha_background_overlay_hover_color_b_stop":{"unit":"%","size":100,"sizes":[]},"_ha_background_overlay_hover_color_b_stop_tablet":{"unit":"%"},"_ha_background_overlay_hover_color_b_stop_mobile":{"unit":"%"},"_ha_background_overlay_hover_gradient_type":"linear","_ha_background_overlay_hover_gradient_angle":{"unit":"deg","size":180,"sizes":[]},"_ha_background_overlay_hover_gradient_angle_tablet":{"unit":"deg"},"_ha_background_overlay_hover_gradient_angle_mobile":{"unit":"deg"},"_ha_background_overlay_hover_gradient_position":"center center","_ha_background_overlay_hover_gradient_position_tablet":"","_ha_background_overlay_hover_gradient_position_mobile":"","_ha_background_overlay_hover_image":{"url":"","id":"","size":""},"_ha_background_overlay_hover_image_tablet":{"url":"","id":"","size":""},"_ha_background_overlay_hover_image_mobile":{"url":"","id":"","size":""},"_ha_background_overlay_hover_position":"","_ha_background_overlay_hover_position_tablet":"","_ha_background_overlay_hover_position_mobile":"","_ha_background_overlay_hover_xpos":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_hover_xpos_tablet":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_hover_xpos_mobile":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_hover_ypos":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_hover_ypos_tablet":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_hover_ypos_mobile":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_hover_attachment":"","_ha_background_overlay_hover_repeat":"","_ha_background_overlay_hover_repeat_tablet":"","_ha_background_overlay_hover_repeat_mobile":"","_ha_background_overlay_hover_size":"","_ha_background_overlay_hover_size_tablet":"","_ha_background_overlay_hover_size_mobile":"","_ha_background_overlay_hover_bg_width":{"unit":"%","size":100,"sizes":[]},"_ha_background_overlay_hover_bg_width_tablet":{"unit":"px","size":"","sizes":[]},"_ha_background_overlay_hover_bg_width_mobile":{"unit":"px","size":"","sizes":[]},"_ha_background_overlay_hover_video_link":"","_ha_background_overlay_hover_video_start":"","_ha_background_overlay_hover_video_end":"","_ha_background_overlay_hover_play_once":"","_ha_background_overlay_hover_play_on_mobile":"","_ha_background_overlay_hover_privacy_mode":"","_ha_background_overlay_hover_video_fallback":{"url":"","id":"","size":""},"_ha_background_overlay_hover_slideshow_gallery":[],"_ha_background_overlay_hover_slideshow_loop":"yes","_ha_background_overlay_hover_slideshow_slide_duration":5000,"_ha_background_overlay_hover_slideshow_slide_transition":"fade","_ha_background_overlay_hover_slideshow_transition_duration":500,"_ha_background_overlay_hover_slideshow_background_size":"","_ha_background_overlay_hover_slideshow_background_size_tablet":"","_ha_background_overlay_hover_slideshow_background_size_mobile":"","_ha_background_overlay_hover_slideshow_background_position":"","_ha_background_overlay_hover_slideshow_background_position_tablet":"","_ha_background_overlay_hover_slideshow_background_position_mobile":"","_ha_background_overlay_hover_slideshow_lazyload":"","_ha_background_overlay_hover_slideshow_ken_burns":"","_ha_background_overlay_hover_slideshow_ken_burns_zoom_direction":"in","_ha_background_overlay_hover_opacity":{"unit":"px","size":0.5,"sizes":[]},"_ha_css_filters_hover_css_filter":"","_ha_css_filters_hover_blur":{"unit":"px","size":0,"sizes":[]},"_ha_css_filters_hover_brightness":{"unit":"px","size":100,"sizes":[]},"_ha_css_filters_hover_contrast":{"unit":"px","size":100,"sizes":[]},"_ha_css_filters_hover_saturate":{"unit":"px","size":100,"sizes":[]},"_ha_css_filters_hover_hue":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_hover_transition":{"unit":"px","size":0.3,"sizes":[]},"_border_border":"","_border_width":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_width_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_width_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_color":"","_border_radius":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_radius_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_radius_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_box_shadow_box_shadow_type":"","_box_shadow_box_shadow":{"horizontal":0,"vertical":0,"blur":10,"spread":0,"color":"rgba(0,0,0,0.5)"},"_box_shadow_box_shadow_position":" ","_border_hover_border":"","_border_hover_width":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_hover_width_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_hover_width_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_hover_color":"","_border_radius_hover":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_radius_hover_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_radius_hover_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_box_shadow_hover_box_shadow_type":"","_box_shadow_hover_box_shadow":{"horizontal":0,"vertical":0,"blur":10,"spread":0,"color":"rgba(0,0,0,0.5)"},"_box_shadow_hover_box_shadow_position":" ","_border_hover_transition":{"unit":"px","size":"","sizes":[]},"_mask_switch":"","_mask_shape":"circle","_mask_image":{"url":"","id":"","size":""},"_mask_notice":"","_mask_size":"contain","_mask_size_tablet":"","_mask_size_mobile":"","_mask_size_scale":{"unit":"%","size":100,"sizes":[]},"_mask_size_scale_tablet":{"unit":"px","size":"","sizes":[]},"_mask_size_scale_mobile":{"unit":"px","size":"","sizes":[]},"_mask_position":"center center","_mask_position_tablet":"","_mask_position_mobile":"","_mask_position_x":{"unit":"%","size":0,"sizes":[]},"_mask_position_x_tablet":{"unit":"px","size":"","sizes":[]},"_mask_position_x_mobile":{"unit":"px","size":"","sizes":[]},"_mask_position_y":{"unit":"%","size":0,"sizes":[]},"_mask_position_y_tablet":{"unit":"px","size":"","sizes":[]},"_mask_position_y_mobile":{"unit":"px","size":"","sizes":[]},"_mask_repeat":"no-repeat","_mask_repeat_tablet":"","_mask_repeat_mobile":"","hide_desktop":"","hide_tablet":"","hide_mobile":"","ma_el_position_type":"","ma_el_position_type_tablet":"","ma_el_position_type_mobile":"","ma_el_position_top":{"unit":"px","size":"","sizes":[]},"ma_el_position_top_tablet":{"unit":"px","size":"","sizes":[]},"ma_el_position_top_mobile":{"unit":"px","size":"","sizes":[]},"ma_el_position_right":{"unit":"px","size":"","sizes":[]},"ma_el_position_right_tablet":{"unit":"px","size":"","sizes":[]},"ma_el_position_right_mobile":{"unit":"px","size":"","sizes":[]},"ma_el_position_bottom":{"unit":"px","size":"","sizes":[]},"ma_el_position_bottom_tablet":{"unit":"px","size":"","sizes":[]},"ma_el_position_bottom_mobile":{"unit":"px","size":"","sizes":[]},"ma_el_position_left":{"unit":"px","size":"","sizes":[]},"ma_el_position_left_tablet":{"unit":"px","size":"","sizes":[]},"ma_el_position_left_mobile":{"unit":"px","size":"","sizes":[]},"ma_el_position_from_center":{"unit":"px","size":"","sizes":[]},"ma_el_position_from_center_tablet":{"unit":"px","size":"","sizes":[]},"ma_el_position_from_center_mobile":{"unit":"px","size":"","sizes":[]},"ma_el_position_zindex":"","ma_el_position_zindex_tablet":"","ma_el_position_zindex_mobile":"","ma_el_max_width":{"unit":"px","size":"","sizes":[]},"ma_el_max_width_tablet":{"unit":"px","size":"","sizes":[]},"ma_el_max_width_mobile":{"unit":"px","size":"","sizes":[]},"ma_el_max_height":{"unit":"px","size":"","sizes":[]},"ma_el_max_height_tablet":{"unit":"px","size":"","sizes":[]},"ma_el_max_height_mobile":{"unit":"px","size":"","sizes":[]},"ma_el_min_width":{"unit":"px","size":"","sizes":[]},"ma_el_min_width_tablet":{"unit":"px","size":"","sizes":[]},"ma_el_min_width_mobile":{"unit":"px","size":"","sizes":[]},"ma_el_min_height":{"unit":"px","size":"","sizes":[]},"ma_el_min_height_tablet":{"unit":"px","size":"","sizes":[]},"ma_el_min_height_mobile":{"unit":"px","size":"","sizes":[]},"custom_css":""},"defaultEditSettings":{"defaultEditRoute":"content"},"elements":[],"widgetType":"image","htmlCache":"\t\t\n\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\n\t\t","editSettings":{"defaultEditRoute":"content","panel":{"activeTab":"content","activeSection":"section_image"}}}]}](https://www.alleviatepainclinic.com/wp-content/uploads/2024/05/Downloader.la-6647086e4615b.jpg)
![{"type":"elementor","siteurl":"http:\/\/alleviatepainclinic.com\/wp-json\/","elements":[{"id":"e469b3d","elType":"widget","isInner":false,"isLocked":false,"settings":{"image":{"url":"http:\/\/alleviatepainclinic.com\/wp-content\/uploads\/2024\/05\/Downloader.la-6647086e4615b.jpg","id":18300,"size":"","alt":"","source":"library"},"_margin":{"unit":"px","top":"20","right":"0","bottom":"0","left":"0","isLinked":false},"ha_advanced_tooltip_content":"I am a tooltip","image_size":"large","image_custom_dimension":{"width":"","height":""},"caption_source":"none","caption":"","link_to":"none","link":{"url":"","is_external":"","nofollow":"","custom_attributes":""},"open_lightbox":"default","align":"","align_tablet":"","align_mobile":"","width":{"unit":"%","size":"","sizes":[]},"width_tablet":{"unit":"%","size":"","sizes":[]},"width_mobile":{"unit":"%","size":"","sizes":[]},"space":{"unit":"%","size":"","sizes":[]},"space_tablet":{"unit":"%","size":"","sizes":[]},"space_mobile":{"unit":"%","size":"","sizes":[]},"height":{"unit":"px","size":"","sizes":[]},"height_tablet":{"unit":"px","size":"","sizes":[]},"height_mobile":{"unit":"px","size":"","sizes":[]},"object-fit":"","object-fit_tablet":"","object-fit_mobile":"","object-position":"center center","object-position_tablet":"","object-position_mobile":"","opacity":{"unit":"px","size":"","sizes":[]},"css_filters_css_filter":"","css_filters_blur":{"unit":"px","size":0,"sizes":[]},"css_filters_brightness":{"unit":"px","size":100,"sizes":[]},"css_filters_contrast":{"unit":"px","size":100,"sizes":[]},"css_filters_saturate":{"unit":"px","size":100,"sizes":[]},"css_filters_hue":{"unit":"px","size":0,"sizes":[]},"opacity_hover":{"unit":"px","size":"","sizes":[]},"css_filters_hover_css_filter":"","css_filters_hover_blur":{"unit":"px","size":0,"sizes":[]},"css_filters_hover_brightness":{"unit":"px","size":100,"sizes":[]},"css_filters_hover_contrast":{"unit":"px","size":100,"sizes":[]},"css_filters_hover_saturate":{"unit":"px","size":100,"sizes":[]},"css_filters_hover_hue":{"unit":"px","size":0,"sizes":[]},"background_hover_transition":{"unit":"px","size":"","sizes":[]},"hover_animation":"","image_border_border":"","image_border_width":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"image_border_width_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"image_border_width_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"image_border_color":"","image_border_radius":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"image_border_radius_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"image_border_radius_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"image_box_shadow_box_shadow_type":"","image_box_shadow_box_shadow":{"horizontal":0,"vertical":0,"blur":10,"spread":0,"color":"rgba(0,0,0,0.5)"},"caption_align":"","caption_align_tablet":"","caption_align_mobile":"","text_color":"","caption_background_color":"","caption_typography_typography":"","caption_typography_font_family":"","caption_typography_font_size":{"unit":"px","size":"","sizes":[]},"caption_typography_font_size_tablet":{"unit":"px","size":"","sizes":[]},"caption_typography_font_size_mobile":{"unit":"px","size":"","sizes":[]},"caption_typography_font_weight":"","caption_typography_text_transform":"","caption_typography_font_style":"","caption_typography_text_decoration":"","caption_typography_line_height":{"unit":"px","size":"","sizes":[]},"caption_typography_line_height_tablet":{"unit":"em","size":"","sizes":[]},"caption_typography_line_height_mobile":{"unit":"em","size":"","sizes":[]},"caption_typography_letter_spacing":{"unit":"px","size":"","sizes":[]},"caption_typography_letter_spacing_tablet":{"unit":"px","size":"","sizes":[]},"caption_typography_letter_spacing_mobile":{"unit":"px","size":"","sizes":[]},"caption_typography_word_spacing":{"unit":"px","size":"","sizes":[]},"caption_typography_word_spacing_tablet":{"unit":"em","size":"","sizes":[]},"caption_typography_word_spacing_mobile":{"unit":"em","size":"","sizes":[]},"caption_text_shadow_text_shadow_type":"","caption_text_shadow_text_shadow":{"horizontal":0,"vertical":0,"blur":10,"color":"rgba(0,0,0,0.3)"},"caption_space":{"unit":"px","size":"","sizes":[]},"caption_space_tablet":{"unit":"px","size":"","sizes":[]},"caption_space_mobile":{"unit":"px","size":"","sizes":[]},"_title":"","_margin_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_margin_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_padding":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_padding_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_padding_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_element_width":"","_element_width_tablet":"","_element_width_mobile":"","_element_custom_width":{"unit":"%","size":"","sizes":[]},"_element_custom_width_tablet":{"unit":"px","size":"","sizes":[]},"_element_custom_width_mobile":{"unit":"px","size":"","sizes":[]},"_flex_align_self":"","_flex_align_self_tablet":"","_flex_align_self_mobile":"","_flex_order":"","_flex_order_tablet":"","_flex_order_mobile":"","_flex_order_custom":"","_flex_order_custom_tablet":"","_flex_order_custom_mobile":"","_flex_size":"","_flex_size_tablet":"","_flex_size_mobile":"","_flex_grow":1,"_flex_grow_tablet":"","_flex_grow_mobile":"","_flex_shrink":1,"_flex_shrink_tablet":"","_flex_shrink_mobile":"","_element_vertical_align":"","_element_vertical_align_tablet":"","_element_vertical_align_mobile":"","_position":"","_offset_orientation_h":"start","_offset_x":{"unit":"px","size":0,"sizes":[]},"_offset_x_tablet":{"unit":"px","size":"","sizes":[]},"_offset_x_mobile":{"unit":"px","size":"","sizes":[]},"_offset_x_end":{"unit":"px","size":0,"sizes":[]},"_offset_x_end_tablet":{"unit":"px","size":"","sizes":[]},"_offset_x_end_mobile":{"unit":"px","size":"","sizes":[]},"_offset_orientation_v":"start","_offset_y":{"unit":"px","size":0,"sizes":[]},"_offset_y_tablet":{"unit":"px","size":"","sizes":[]},"_offset_y_mobile":{"unit":"px","size":"","sizes":[]},"_offset_y_end":{"unit":"px","size":0,"sizes":[]},"_offset_y_end_tablet":{"unit":"px","size":"","sizes":[]},"_offset_y_end_mobile":{"unit":"px","size":"","sizes":[]},"_z_index":"","_z_index_tablet":"","_z_index_mobile":"","_element_id":"","_css_classes":"","ha_floating_fx":"","ha_floating_fx_translate_toggle":"","ha_floating_fx_translate_x":{"unit":"px","size":"","sizes":{"from":0,"to":5}},"ha_floating_fx_translate_y":{"unit":"px","size":"","sizes":{"from":0,"to":5}},"ha_floating_fx_translate_duration":{"unit":"px","size":1000,"sizes":[]},"ha_floating_fx_translate_delay":{"unit":"px","size":"","sizes":[]},"ha_floating_fx_rotate_toggle":"","ha_floating_fx_rotate_x":{"unit":"px","size":"","sizes":{"from":0,"to":45}},"ha_floating_fx_rotate_y":{"unit":"px","size":"","sizes":{"from":0,"to":45}},"ha_floating_fx_rotate_z":{"unit":"px","size":"","sizes":{"from":0,"to":45}},"ha_floating_fx_rotate_duration":{"unit":"px","size":1000,"sizes":[]},"ha_floating_fx_rotate_delay":{"unit":"px","size":"","sizes":[]},"ha_floating_fx_scale_toggle":"","ha_floating_fx_scale_x":{"unit":"px","size":"","sizes":{"from":1,"to":1.2}},"ha_floating_fx_scale_y":{"unit":"px","size":"","sizes":{"from":1,"to":1.2}},"ha_floating_fx_scale_duration":{"unit":"px","size":1000,"sizes":[]},"ha_floating_fx_scale_delay":{"unit":"px","size":"","sizes":[]},"ha_element_link":{"url":"","is_external":"","nofollow":"","custom_attributes":""},"ha_transform_fx":"","ha_transform_fx_translate_toggle":"","ha_transform_fx_translate_x":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_x_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_x_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_y":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_y_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_y_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_toggle":"","ha_transform_fx_rotate_mode":"loose","ha_transform_fx_rotate_x":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_x_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_x_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_y":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_y_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_y_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_z":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_z_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_z_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_scale_toggle":"","ha_transform_fx_scale_mode":"loose","ha_transform_fx_scale_x":{"unit":"px","size":1,"sizes":[]},"ha_transform_fx_scale_x_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_scale_x_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_scale_y":{"unit":"px","size":1,"sizes":[]},"ha_transform_fx_scale_y_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_scale_y_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_toggle":"","ha_transform_fx_skew_x":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_x_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_x_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_y":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_y_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_y_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_toggle_hover":"","ha_transform_fx_translate_x_hover":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_x_hover_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_x_hover_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_y_hover":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_y_hover_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_translate_y_hover_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_toggle_hover":"","ha_transform_fx_rotate_mode_hover":"loose","ha_transform_fx_rotate_x_hover":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_x_hover_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_x_hover_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_y_hover":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_y_hover_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_y_hover_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_z_hover":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_z_hover_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_rotate_z_hover_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_scale_toggle_hover":"","ha_transform_fx_scale_mode_hover":"loose","ha_transform_fx_scale_x_hover":{"unit":"px","size":1,"sizes":[]},"ha_transform_fx_scale_x_hover_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_scale_x_hover_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_scale_y_hover":{"unit":"px","size":1,"sizes":[]},"ha_transform_fx_scale_y_hover_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_scale_y_hover_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_toggle_hover":"","ha_transform_fx_skew_x_hover":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_x_hover_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_x_hover_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_y_hover":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_y_hover_tablet":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_skew_y_hover_mobile":{"unit":"px","size":"","sizes":[]},"ha_transform_fx_transition_duration":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_enable":"","ha_advanced_tooltip_position":"top","ha_advanced_tooltip_position_tablet":"","ha_advanced_tooltip_position_mobile":"","ha_advanced_tooltip_animation":"","ha_advanced_tooltip_duration":1000,"ha_advanced_tooltip_arrow":"true","ha_advanced_tooltip_trigger":"hover","ha_advanced_tooltip_distance":{"unit":"px","size":"0","sizes":[]},"ha_advanced_tooltip_distance_tablet":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_distance_mobile":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_align":"center","ha_advanced_tooltip_align_tablet":"","ha_advanced_tooltip_align_mobile":"","ha_advanced_tooltip_width":{"unit":"px","size":"120","sizes":[]},"ha_advanced_tooltip_width_tablet":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_width_mobile":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_arrow_size":{"unit":"px","size":"5","sizes":[]},"ha_advanced_tooltip_arrow_size_tablet":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_arrow_size_mobile":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_typography_typography":"yes","ha_advanced_tooltip_typography_font_family":"Nunito","ha_advanced_tooltip_typography_font_size":{"unit":"px","size":"14","sizes":[]},"ha_advanced_tooltip_typography_font_size_tablet":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_typography_font_size_mobile":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_typography_font_weight":"500","ha_advanced_tooltip_typography_text_transform":"","ha_advanced_tooltip_typography_font_style":"","ha_advanced_tooltip_typography_text_decoration":"","ha_advanced_tooltip_typography_line_height":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_typography_line_height_tablet":{"unit":"em","size":"","sizes":[]},"ha_advanced_tooltip_typography_line_height_mobile":{"unit":"em","size":"","sizes":[]},"ha_advanced_tooltip_typography_letter_spacing":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_typography_letter_spacing_tablet":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_typography_letter_spacing_mobile":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_typography_word_spacing":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_typography_word_spacing_tablet":{"unit":"em","size":"","sizes":[]},"ha_advanced_tooltip_typography_word_spacing_mobile":{"unit":"em","size":"","sizes":[]},"ha_advanced_tooltip_title_section_bg_color_background":"","ha_advanced_tooltip_title_section_bg_color_color":"","ha_advanced_tooltip_title_section_bg_color_color_stop":{"unit":"%","size":0,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_color_stop_tablet":{"unit":"%"},"ha_advanced_tooltip_title_section_bg_color_color_stop_mobile":{"unit":"%"},"ha_advanced_tooltip_title_section_bg_color_color_b":"#f2295b","ha_advanced_tooltip_title_section_bg_color_color_b_stop":{"unit":"%","size":100,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_color_b_stop_tablet":{"unit":"%"},"ha_advanced_tooltip_title_section_bg_color_color_b_stop_mobile":{"unit":"%"},"ha_advanced_tooltip_title_section_bg_color_gradient_type":"linear","ha_advanced_tooltip_title_section_bg_color_gradient_angle":{"unit":"deg","size":180,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_gradient_angle_tablet":{"unit":"deg"},"ha_advanced_tooltip_title_section_bg_color_gradient_angle_mobile":{"unit":"deg"},"ha_advanced_tooltip_title_section_bg_color_gradient_position":"center center","ha_advanced_tooltip_title_section_bg_color_gradient_position_tablet":"","ha_advanced_tooltip_title_section_bg_color_gradient_position_mobile":"","ha_advanced_tooltip_title_section_bg_color_image":{"url":"","id":"","size":""},"ha_advanced_tooltip_title_section_bg_color_image_tablet":{"url":"","id":"","size":""},"ha_advanced_tooltip_title_section_bg_color_image_mobile":{"url":"","id":"","size":""},"ha_advanced_tooltip_title_section_bg_color_position":"","ha_advanced_tooltip_title_section_bg_color_position_tablet":"","ha_advanced_tooltip_title_section_bg_color_position_mobile":"","ha_advanced_tooltip_title_section_bg_color_xpos":{"unit":"px","size":0,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_xpos_tablet":{"unit":"px","size":0,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_xpos_mobile":{"unit":"px","size":0,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_ypos":{"unit":"px","size":0,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_ypos_tablet":{"unit":"px","size":0,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_ypos_mobile":{"unit":"px","size":0,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_attachment":"","ha_advanced_tooltip_title_section_bg_color_repeat":"","ha_advanced_tooltip_title_section_bg_color_repeat_tablet":"","ha_advanced_tooltip_title_section_bg_color_repeat_mobile":"","ha_advanced_tooltip_title_section_bg_color_size":"","ha_advanced_tooltip_title_section_bg_color_size_tablet":"","ha_advanced_tooltip_title_section_bg_color_size_mobile":"","ha_advanced_tooltip_title_section_bg_color_bg_width":{"unit":"%","size":100,"sizes":[]},"ha_advanced_tooltip_title_section_bg_color_bg_width_tablet":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_title_section_bg_color_bg_width_mobile":{"unit":"px","size":"","sizes":[]},"ha_advanced_tooltip_title_section_bg_color_video_link":"","ha_advanced_tooltip_title_section_bg_color_video_start":"","ha_advanced_tooltip_title_section_bg_color_video_end":"","ha_advanced_tooltip_title_section_bg_color_play_once":"","ha_advanced_tooltip_title_section_bg_color_play_on_mobile":"","ha_advanced_tooltip_title_section_bg_color_privacy_mode":"","ha_advanced_tooltip_title_section_bg_color_video_fallback":{"url":"","id":"","size":""},"ha_advanced_tooltip_title_section_bg_color_slideshow_gallery":[],"ha_advanced_tooltip_title_section_bg_color_slideshow_loop":"yes","ha_advanced_tooltip_title_section_bg_color_slideshow_slide_duration":5000,"ha_advanced_tooltip_title_section_bg_color_slideshow_slide_transition":"fade","ha_advanced_tooltip_title_section_bg_color_slideshow_transition_duration":500,"ha_advanced_tooltip_title_section_bg_color_slideshow_background_size":"","ha_advanced_tooltip_title_section_bg_color_slideshow_background_size_tablet":"","ha_advanced_tooltip_title_section_bg_color_slideshow_background_size_mobile":"","ha_advanced_tooltip_title_section_bg_color_slideshow_background_position":"","ha_advanced_tooltip_title_section_bg_color_slideshow_background_position_tablet":"","ha_advanced_tooltip_title_section_bg_color_slideshow_background_position_mobile":"","ha_advanced_tooltip_title_section_bg_color_slideshow_lazyload":"","ha_advanced_tooltip_title_section_bg_color_slideshow_ken_burns":"","ha_advanced_tooltip_title_section_bg_color_slideshow_ken_burns_zoom_direction":"in","ha_advanced_tooltip_background_color":"#000000","ha_advanced_tooltip_color":"#ffffff","ha_advanced_tooltip_border_border":"","ha_advanced_tooltip_border_width":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"ha_advanced_tooltip_border_width_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"ha_advanced_tooltip_border_width_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"ha_advanced_tooltip_border_color":"","ha_advanced_tooltip_border_radius":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"ha_advanced_tooltip_border_radius_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"ha_advanced_tooltip_border_radius_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"ha_advanced_tooltip_padding":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"ha_advanced_tooltip_padding_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"ha_advanced_tooltip_padding_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"ha_advanced_tooltip_box_shadow_box_shadow_type":"","ha_advanced_tooltip_box_shadow_box_shadow":{"horizontal":0,"vertical":0,"blur":10,"spread":0,"color":"rgba(0,0,0,0.5)"},"ha_advanced_tooltip_box_shadow_box_shadow_position":" ","jltma_section_element_link":{"url":"","is_external":"","nofollow":"","custom_attributes":""},"_animation":"","_animation_tablet":"","_animation_mobile":"","animation_duration":"","_animation_delay":"","_transform_rotate_popover":"","_transform_rotateZ_effect":{"unit":"px","size":"","sizes":[]},"_transform_rotateZ_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateZ_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_rotate_3d":"","_transform_rotateX_effect":{"unit":"px","size":"","sizes":[]},"_transform_rotateX_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateX_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_rotateY_effect":{"unit":"px","size":"","sizes":[]},"_transform_rotateY_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateY_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_perspective_effect":{"unit":"px","size":"","sizes":[]},"_transform_perspective_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_perspective_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_translate_popover":"","_transform_translateX_effect":{"unit":"px","size":"","sizes":[]},"_transform_translateX_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_translateX_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scale_popover":"","_transform_keep_proportions":"yes","_transform_scale_effect":{"unit":"px","size":"","sizes":[]},"_transform_scale_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scale_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_mobile":{"unit":"px","size":"","sizes":[]},"_transform_skew_popover":"","_transform_skewX_effect":{"unit":"px","size":"","sizes":[]},"_transform_skewX_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_skewX_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_skewY_effect":{"unit":"px","size":"","sizes":[]},"_transform_skewY_effect_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_skewY_effect_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_flipX_effect":"","_transform_flipY_effect":"","_transform_rotate_popover_hover":"","_transform_rotateZ_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_rotateZ_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateZ_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_rotate_3d_hover":"","_transform_rotateX_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_rotateX_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateX_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_rotateY_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_rotateY_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_rotateY_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_perspective_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_perspective_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_perspective_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_translate_popover_hover":"","_transform_translateX_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_translateX_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_translateX_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_translateY_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scale_popover_hover":"","_transform_keep_proportions_hover":"yes","_transform_scale_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_scale_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scale_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scaleX_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_hover_tablet":{"unit":"px","size":"","sizes":[]},"_transform_scaleY_effect_hover_mobile":{"unit":"px","size":"","sizes":[]},"_transform_skew_popover_hover":"","_transform_skewX_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_skewX_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_skewX_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_skewY_effect_hover":{"unit":"px","size":"","sizes":[]},"_transform_skewY_effect_hover_tablet":{"unit":"deg","size":"","sizes":[]},"_transform_skewY_effect_hover_mobile":{"unit":"deg","size":"","sizes":[]},"_transform_flipX_effect_hover":"","_transform_flipY_effect_hover":"","_transform_transition_hover":{"unit":"px","size":"","sizes":[]},"motion_fx_transform_x_anchor_point":"","motion_fx_transform_x_anchor_point_tablet":"","motion_fx_transform_x_anchor_point_mobile":"","motion_fx_transform_y_anchor_point":"","motion_fx_transform_y_anchor_point_tablet":"","motion_fx_transform_y_anchor_point_mobile":"","_background_background":"","_background_color":"","_background_color_stop":{"unit":"%","size":0,"sizes":[]},"_background_color_stop_tablet":{"unit":"%"},"_background_color_stop_mobile":{"unit":"%"},"_background_color_b":"#f2295b","_background_color_b_stop":{"unit":"%","size":100,"sizes":[]},"_background_color_b_stop_tablet":{"unit":"%"},"_background_color_b_stop_mobile":{"unit":"%"},"_background_gradient_type":"linear","_background_gradient_angle":{"unit":"deg","size":180,"sizes":[]},"_background_gradient_angle_tablet":{"unit":"deg"},"_background_gradient_angle_mobile":{"unit":"deg"},"_background_gradient_position":"center center","_background_gradient_position_tablet":"","_background_gradient_position_mobile":"","_background_image":{"url":"","id":"","size":""},"_background_image_tablet":{"url":"","id":"","size":""},"_background_image_mobile":{"url":"","id":"","size":""},"_background_position":"","_background_position_tablet":"","_background_position_mobile":"","_background_xpos":{"unit":"px","size":0,"sizes":[]},"_background_xpos_tablet":{"unit":"px","size":0,"sizes":[]},"_background_xpos_mobile":{"unit":"px","size":0,"sizes":[]},"_background_ypos":{"unit":"px","size":0,"sizes":[]},"_background_ypos_tablet":{"unit":"px","size":0,"sizes":[]},"_background_ypos_mobile":{"unit":"px","size":0,"sizes":[]},"_background_attachment":"","_background_repeat":"","_background_repeat_tablet":"","_background_repeat_mobile":"","_background_size":"","_background_size_tablet":"","_background_size_mobile":"","_background_bg_width":{"unit":"%","size":100,"sizes":[]},"_background_bg_width_tablet":{"unit":"px","size":"","sizes":[]},"_background_bg_width_mobile":{"unit":"px","size":"","sizes":[]},"_background_video_link":"","_background_video_start":"","_background_video_end":"","_background_play_once":"","_background_play_on_mobile":"","_background_privacy_mode":"","_background_video_fallback":{"url":"","id":"","size":""},"_background_slideshow_gallery":[],"_background_slideshow_loop":"yes","_background_slideshow_slide_duration":5000,"_background_slideshow_slide_transition":"fade","_background_slideshow_transition_duration":500,"_background_slideshow_background_size":"","_background_slideshow_background_size_tablet":"","_background_slideshow_background_size_mobile":"","_background_slideshow_background_position":"","_background_slideshow_background_position_tablet":"","_background_slideshow_background_position_mobile":"","_background_slideshow_lazyload":"","_background_slideshow_ken_burns":"","_background_slideshow_ken_burns_zoom_direction":"in","_background_hover_background":"","_background_hover_color":"","_background_hover_color_stop":{"unit":"%","size":0,"sizes":[]},"_background_hover_color_stop_tablet":{"unit":"%"},"_background_hover_color_stop_mobile":{"unit":"%"},"_background_hover_color_b":"#f2295b","_background_hover_color_b_stop":{"unit":"%","size":100,"sizes":[]},"_background_hover_color_b_stop_tablet":{"unit":"%"},"_background_hover_color_b_stop_mobile":{"unit":"%"},"_background_hover_gradient_type":"linear","_background_hover_gradient_angle":{"unit":"deg","size":180,"sizes":[]},"_background_hover_gradient_angle_tablet":{"unit":"deg"},"_background_hover_gradient_angle_mobile":{"unit":"deg"},"_background_hover_gradient_position":"center center","_background_hover_gradient_position_tablet":"","_background_hover_gradient_position_mobile":"","_background_hover_image":{"url":"","id":"","size":""},"_background_hover_image_tablet":{"url":"","id":"","size":""},"_background_hover_image_mobile":{"url":"","id":"","size":""},"_background_hover_position":"","_background_hover_position_tablet":"","_background_hover_position_mobile":"","_background_hover_xpos":{"unit":"px","size":0,"sizes":[]},"_background_hover_xpos_tablet":{"unit":"px","size":0,"sizes":[]},"_background_hover_xpos_mobile":{"unit":"px","size":0,"sizes":[]},"_background_hover_ypos":{"unit":"px","size":0,"sizes":[]},"_background_hover_ypos_tablet":{"unit":"px","size":0,"sizes":[]},"_background_hover_ypos_mobile":{"unit":"px","size":0,"sizes":[]},"_background_hover_attachment":"","_background_hover_repeat":"","_background_hover_repeat_tablet":"","_background_hover_repeat_mobile":"","_background_hover_size":"","_background_hover_size_tablet":"","_background_hover_size_mobile":"","_background_hover_bg_width":{"unit":"%","size":100,"sizes":[]},"_background_hover_bg_width_tablet":{"unit":"px","size":"","sizes":[]},"_background_hover_bg_width_mobile":{"unit":"px","size":"","sizes":[]},"_background_hover_video_link":"","_background_hover_video_start":"","_background_hover_video_end":"","_background_hover_play_once":"","_background_hover_play_on_mobile":"","_background_hover_privacy_mode":"","_background_hover_video_fallback":{"url":"","id":"","size":""},"_background_hover_slideshow_gallery":[],"_background_hover_slideshow_loop":"yes","_background_hover_slideshow_slide_duration":5000,"_background_hover_slideshow_slide_transition":"fade","_background_hover_slideshow_transition_duration":500,"_background_hover_slideshow_background_size":"","_background_hover_slideshow_background_size_tablet":"","_background_hover_slideshow_background_size_mobile":"","_background_hover_slideshow_background_position":"","_background_hover_slideshow_background_position_tablet":"","_background_hover_slideshow_background_position_mobile":"","_background_hover_slideshow_lazyload":"","_background_hover_slideshow_ken_burns":"","_background_hover_slideshow_ken_burns_zoom_direction":"in","_background_hover_transition":{"unit":"px","size":"","sizes":[]},"jltma_enable_glassmorphism_effect":"no","jltma_glass_effect_blur_value":20,"_ha_background_overlay_background":"","_ha_background_overlay_color":"","_ha_background_overlay_color_stop":{"unit":"%","size":0,"sizes":[]},"_ha_background_overlay_color_stop_tablet":{"unit":"%"},"_ha_background_overlay_color_stop_mobile":{"unit":"%"},"_ha_background_overlay_color_b":"#f2295b","_ha_background_overlay_color_b_stop":{"unit":"%","size":100,"sizes":[]},"_ha_background_overlay_color_b_stop_tablet":{"unit":"%"},"_ha_background_overlay_color_b_stop_mobile":{"unit":"%"},"_ha_background_overlay_gradient_type":"linear","_ha_background_overlay_gradient_angle":{"unit":"deg","size":180,"sizes":[]},"_ha_background_overlay_gradient_angle_tablet":{"unit":"deg"},"_ha_background_overlay_gradient_angle_mobile":{"unit":"deg"},"_ha_background_overlay_gradient_position":"center center","_ha_background_overlay_gradient_position_tablet":"","_ha_background_overlay_gradient_position_mobile":"","_ha_background_overlay_image":{"url":"","id":"","size":""},"_ha_background_overlay_image_tablet":{"url":"","id":"","size":""},"_ha_background_overlay_image_mobile":{"url":"","id":"","size":""},"_ha_background_overlay_position":"","_ha_background_overlay_position_tablet":"","_ha_background_overlay_position_mobile":"","_ha_background_overlay_xpos":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_xpos_tablet":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_xpos_mobile":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_ypos":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_ypos_tablet":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_ypos_mobile":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_attachment":"","_ha_background_overlay_repeat":"","_ha_background_overlay_repeat_tablet":"","_ha_background_overlay_repeat_mobile":"","_ha_background_overlay_size":"","_ha_background_overlay_size_tablet":"","_ha_background_overlay_size_mobile":"","_ha_background_overlay_bg_width":{"unit":"%","size":100,"sizes":[]},"_ha_background_overlay_bg_width_tablet":{"unit":"px","size":"","sizes":[]},"_ha_background_overlay_bg_width_mobile":{"unit":"px","size":"","sizes":[]},"_ha_background_overlay_video_link":"","_ha_background_overlay_video_start":"","_ha_background_overlay_video_end":"","_ha_background_overlay_play_once":"","_ha_background_overlay_play_on_mobile":"","_ha_background_overlay_privacy_mode":"","_ha_background_overlay_video_fallback":{"url":"","id":"","size":""},"_ha_background_overlay_slideshow_gallery":[],"_ha_background_overlay_slideshow_loop":"yes","_ha_background_overlay_slideshow_slide_duration":5000,"_ha_background_overlay_slideshow_slide_transition":"fade","_ha_background_overlay_slideshow_transition_duration":500,"_ha_background_overlay_slideshow_background_size":"","_ha_background_overlay_slideshow_background_size_tablet":"","_ha_background_overlay_slideshow_background_size_mobile":"","_ha_background_overlay_slideshow_background_position":"","_ha_background_overlay_slideshow_background_position_tablet":"","_ha_background_overlay_slideshow_background_position_mobile":"","_ha_background_overlay_slideshow_lazyload":"","_ha_background_overlay_slideshow_ken_burns":"","_ha_background_overlay_slideshow_ken_burns_zoom_direction":"in","_ha_background_overlay_opacity":{"unit":"px","size":0.5,"sizes":[]},"_ha_css_filters_css_filter":"","_ha_css_filters_blur":{"unit":"px","size":0,"sizes":[]},"_ha_css_filters_brightness":{"unit":"px","size":100,"sizes":[]},"_ha_css_filters_contrast":{"unit":"px","size":100,"sizes":[]},"_ha_css_filters_saturate":{"unit":"px","size":100,"sizes":[]},"_ha_css_filters_hue":{"unit":"px","size":0,"sizes":[]},"_ha_overlay_blend_mode":"","_ha_background_overlay_hover_background":"","_ha_background_overlay_hover_color":"","_ha_background_overlay_hover_color_stop":{"unit":"%","size":0,"sizes":[]},"_ha_background_overlay_hover_color_stop_tablet":{"unit":"%"},"_ha_background_overlay_hover_color_stop_mobile":{"unit":"%"},"_ha_background_overlay_hover_color_b":"#f2295b","_ha_background_overlay_hover_color_b_stop":{"unit":"%","size":100,"sizes":[]},"_ha_background_overlay_hover_color_b_stop_tablet":{"unit":"%"},"_ha_background_overlay_hover_color_b_stop_mobile":{"unit":"%"},"_ha_background_overlay_hover_gradient_type":"linear","_ha_background_overlay_hover_gradient_angle":{"unit":"deg","size":180,"sizes":[]},"_ha_background_overlay_hover_gradient_angle_tablet":{"unit":"deg"},"_ha_background_overlay_hover_gradient_angle_mobile":{"unit":"deg"},"_ha_background_overlay_hover_gradient_position":"center center","_ha_background_overlay_hover_gradient_position_tablet":"","_ha_background_overlay_hover_gradient_position_mobile":"","_ha_background_overlay_hover_image":{"url":"","id":"","size":""},"_ha_background_overlay_hover_image_tablet":{"url":"","id":"","size":""},"_ha_background_overlay_hover_image_mobile":{"url":"","id":"","size":""},"_ha_background_overlay_hover_position":"","_ha_background_overlay_hover_position_tablet":"","_ha_background_overlay_hover_position_mobile":"","_ha_background_overlay_hover_xpos":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_hover_xpos_tablet":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_hover_xpos_mobile":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_hover_ypos":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_hover_ypos_tablet":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_hover_ypos_mobile":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_hover_attachment":"","_ha_background_overlay_hover_repeat":"","_ha_background_overlay_hover_repeat_tablet":"","_ha_background_overlay_hover_repeat_mobile":"","_ha_background_overlay_hover_size":"","_ha_background_overlay_hover_size_tablet":"","_ha_background_overlay_hover_size_mobile":"","_ha_background_overlay_hover_bg_width":{"unit":"%","size":100,"sizes":[]},"_ha_background_overlay_hover_bg_width_tablet":{"unit":"px","size":"","sizes":[]},"_ha_background_overlay_hover_bg_width_mobile":{"unit":"px","size":"","sizes":[]},"_ha_background_overlay_hover_video_link":"","_ha_background_overlay_hover_video_start":"","_ha_background_overlay_hover_video_end":"","_ha_background_overlay_hover_play_once":"","_ha_background_overlay_hover_play_on_mobile":"","_ha_background_overlay_hover_privacy_mode":"","_ha_background_overlay_hover_video_fallback":{"url":"","id":"","size":""},"_ha_background_overlay_hover_slideshow_gallery":[],"_ha_background_overlay_hover_slideshow_loop":"yes","_ha_background_overlay_hover_slideshow_slide_duration":5000,"_ha_background_overlay_hover_slideshow_slide_transition":"fade","_ha_background_overlay_hover_slideshow_transition_duration":500,"_ha_background_overlay_hover_slideshow_background_size":"","_ha_background_overlay_hover_slideshow_background_size_tablet":"","_ha_background_overlay_hover_slideshow_background_size_mobile":"","_ha_background_overlay_hover_slideshow_background_position":"","_ha_background_overlay_hover_slideshow_background_position_tablet":"","_ha_background_overlay_hover_slideshow_background_position_mobile":"","_ha_background_overlay_hover_slideshow_lazyload":"","_ha_background_overlay_hover_slideshow_ken_burns":"","_ha_background_overlay_hover_slideshow_ken_burns_zoom_direction":"in","_ha_background_overlay_hover_opacity":{"unit":"px","size":0.5,"sizes":[]},"_ha_css_filters_hover_css_filter":"","_ha_css_filters_hover_blur":{"unit":"px","size":0,"sizes":[]},"_ha_css_filters_hover_brightness":{"unit":"px","size":100,"sizes":[]},"_ha_css_filters_hover_contrast":{"unit":"px","size":100,"sizes":[]},"_ha_css_filters_hover_saturate":{"unit":"px","size":100,"sizes":[]},"_ha_css_filters_hover_hue":{"unit":"px","size":0,"sizes":[]},"_ha_background_overlay_hover_transition":{"unit":"px","size":0.3,"sizes":[]},"_border_border":"","_border_width":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_width_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_width_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_color":"","_border_radius":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_radius_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_radius_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_box_shadow_box_shadow_type":"","_box_shadow_box_shadow":{"horizontal":0,"vertical":0,"blur":10,"spread":0,"color":"rgba(0,0,0,0.5)"},"_box_shadow_box_shadow_position":" ","_border_hover_border":"","_border_hover_width":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_hover_width_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_hover_width_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_hover_color":"","_border_radius_hover":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_radius_hover_tablet":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_border_radius_hover_mobile":{"unit":"px","top":"","right":"","bottom":"","left":"","isLinked":true},"_box_shadow_hover_box_shadow_type":"","_box_shadow_hover_box_shadow":{"horizontal":0,"vertical":0,"blur":10,"spread":0,"color":"rgba(0,0,0,0.5)"},"_box_shadow_hover_box_shadow_position":" ","_border_hover_transition":{"unit":"px","size":"","sizes":[]},"_mask_switch":"","_mask_shape":"circle","_mask_image":{"url":"","id":"","size":""},"_mask_notice":"","_mask_size":"contain","_mask_size_tablet":"","_mask_size_mobile":"","_mask_size_scale":{"unit":"%","size":100,"sizes":[]},"_mask_size_scale_tablet":{"unit":"px","size":"","sizes":[]},"_mask_size_scale_mobile":{"unit":"px","size":"","sizes":[]},"_mask_position":"center center","_mask_position_tablet":"","_mask_position_mobile":"","_mask_position_x":{"unit":"%","size":0,"sizes":[]},"_mask_position_x_tablet":{"unit":"px","size":"","sizes":[]},"_mask_position_x_mobile":{"unit":"px","size":"","sizes":[]},"_mask_position_y":{"unit":"%","size":0,"sizes":[]},"_mask_position_y_tablet":{"unit":"px","size":"","sizes":[]},"_mask_position_y_mobile":{"unit":"px","size":"","sizes":[]},"_mask_repeat":"no-repeat","_mask_repeat_tablet":"","_mask_repeat_mobile":"","hide_desktop":"","hide_tablet":"","hide_mobile":"","ma_el_position_type":"","ma_el_position_type_tablet":"","ma_el_position_type_mobile":"","ma_el_position_top":{"unit":"px","size":"","sizes":[]},"ma_el_position_top_tablet":{"unit":"px","size":"","sizes":[]},"ma_el_position_top_mobile":{"unit":"px","size":"","sizes":[]},"ma_el_position_right":{"unit":"px","size":"","sizes":[]},"ma_el_position_right_tablet":{"unit":"px","size":"","sizes":[]},"ma_el_position_right_mobile":{"unit":"px","size":"","sizes":[]},"ma_el_position_bottom":{"unit":"px","size":"","sizes":[]},"ma_el_position_bottom_tablet":{"unit":"px","size":"","sizes":[]},"ma_el_position_bottom_mobile":{"unit":"px","size":"","sizes":[]},"ma_el_position_left":{"unit":"px","size":"","sizes":[]},"ma_el_position_left_tablet":{"unit":"px","size":"","sizes":[]},"ma_el_position_left_mobile":{"unit":"px","size":"","sizes":[]},"ma_el_position_from_center":{"unit":"px","size":"","sizes":[]},"ma_el_position_from_center_tablet":{"unit":"px","size":"","sizes":[]},"ma_el_position_from_center_mobile":{"unit":"px","size":"","sizes":[]},"ma_el_position_zindex":"","ma_el_position_zindex_tablet":"","ma_el_position_zindex_mobile":"","ma_el_max_width":{"unit":"px","size":"","sizes":[]},"ma_el_max_width_tablet":{"unit":"px","size":"","sizes":[]},"ma_el_max_width_mobile":{"unit":"px","size":"","sizes":[]},"ma_el_max_height":{"unit":"px","size":"","sizes":[]},"ma_el_max_height_tablet":{"unit":"px","size":"","sizes":[]},"ma_el_max_height_mobile":{"unit":"px","size":"","sizes":[]},"ma_el_min_width":{"unit":"px","size":"","sizes":[]},"ma_el_min_width_tablet":{"unit":"px","size":"","sizes":[]},"ma_el_min_width_mobile":{"unit":"px","size":"","sizes":[]},"ma_el_min_height":{"unit":"px","size":"","sizes":[]},"ma_el_min_height_tablet":{"unit":"px","size":"","sizes":[]},"ma_el_min_height_mobile":{"unit":"px","size":"","sizes":[]},"custom_css":""},"defaultEditSettings":{"defaultEditRoute":"content"},"elements":[],"widgetType":"image","htmlCache":"\t\t\n\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\t\n\t\t","editSettings":{"defaultEditRoute":"content","panel":{"activeTab":"content","activeSection":"section_image"}}}]}](https://www.alleviatepainclinic.com/wp-content/uploads/2024/05/Downloader.la-6647086e4615b.jpg)
FAQs - Chondromalacia Patella
People who are at risk for developing chondromalacia patella include:
- Those who are overweight
- People who have had an injury, fracture, or dislocation related to the kneecap
- Runners, soccer players, bicyclists, and other people who exercise often
- Teenagers and healthy young adults, more often females
Chondromalacia patella often occurs when the undersurface of the kneecap comes in contact with the thigh bone causing swelling and pain. Abnormal knee cap positioning, tightness or weakness of the muscles associated with the knee, too much activity involving the knee, and flat feet may increase the likelihood of chondromalacia patella.
Dull, aching pain that is felt:
- Below the kneecap
- On the sides of the kneecap
A feeling of grinding when the knee is flexed may occur. This can happen:
- Doing knee bends
- Going down stairs
- Running down hill
- Standing up after sitting for awhile
- Blood tests and/or a standard knee X-ray – This may help to rule out some types of arthritis or inflammation.
- MRI scan- A tests that shows details of the knee joint and can reveal many cases of chondromalacia patella.
- Placing of an ice or cold pack to the area for 15-20 minutes, four times daily, for several days. Do not apply ice directly to the skin. Wrap the ice or cold pack with a towel.
- Nonsteroidal anti-inflammatory drugs (NSAIDs) for pain relief. Topical pain medication— These include creams or patches that are applied to the skin to help with soft tissue pain.
- Prescription pain relievers.
- Changing the way you exercise
- Doing exercises to both stretch and strengthen the quadriceps and hamstring muscles
- Losing weight (if you need to)
- Using special shoe inserts and support devices
- Taping to realign the kneecap
- Wearing the right kind of sport or running shoes
Video Spotlight
Blog
Surgery-Free Solutions
Expert Tips for Pain Management
Testimonials
Words From Our Patients
The treatment was very good and the doctor Faraz Ahmed was very kind to the patient and explained clearly the procedure of knee bilateral ha & botox And we were advised to do physiotherapy. We are very much satisfied. We would recommend this alleviate pain clinic.Thank you
Got treatment of Botox and HA for right knee arthritis a month ago and finding good relief from pain. Was treated by Dr Swagtesh Bastia who explained very well about the injections and the treatment was painless. The front desk staff were very kind and very helpful and physiotherapy was also done expertly, overall good experience
Alleviate Pain Management clinic has been a godsend for my mom's knee pain. She has been treated by Dr. Wiquar Ahmed. The attentive staff provided personalised care, and after her treatment, she's feeling remarkably better. Thank you for giving my mom the relief she deserves!
The clinic is super clean with a great OT and most importantly all the staff here are very helpful and considerate. My gratitude to Dr Roshan, the nurses, and support staff - they were always available to assist with any issues post procedure and they even made an extra effort to make a home visit for a follow up check-up. This team here is the perfect example of healing and care with a human touch. Thank you!!!!!
My wife had knee pain I have visited alleviate pain and consulted doc santhoshi now she is able to walk pain free and can do her daily activity than before.the physiotherapist here Dr akhila also helped her with few exercises and the staff here Abdul explained all the procedures well . Thank you PPL can visit here for pain relief





