Epidural Injections
- Home
- Treatments
- Non-Surgical Injections & Blocks
- Epidural Injections
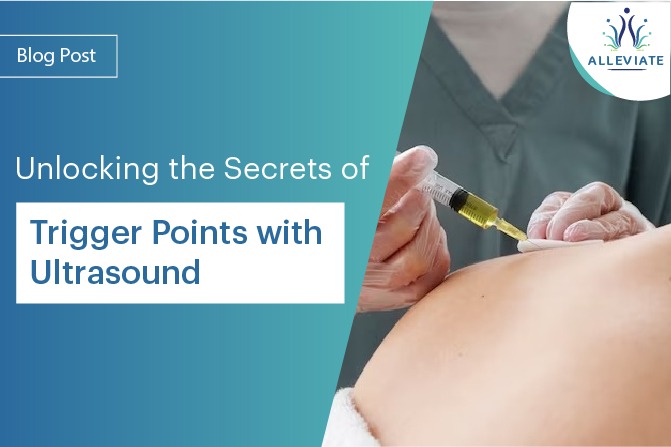
Epidural Injections are a common method of treating inflammation associated with low back related leg pain, or neck related arm pain. In both of these conditions, the spinal nerves become inflamed due to narrowing of the passages where the nerves travel as they pass down or out of the spine.
FAQs - Epidural Injections
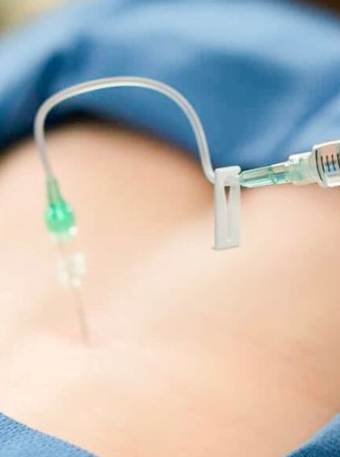
There are three common methods for delivering into the epidural space: the interlaminar, caudal, and transforaminal approaches. All three approaches entail placing a thin needle into position using fluoroscopic (x-ray) guidance. Prior to the injection, contrast dye is used to confirm that the medication is traveling into the desired area. Often, local anesthetic is added along with the steroid to provide temporary pain relief.
An interlaminar epidural injection, often referred to simply as an ‘epidural injection’, involves placing the needle into the back of the epidural space and delivering over a wider area. Similarly, the caudal approach uses the sacral hiatus (a small boney opening just above the tailbone) to allow for needle placement into the very bottom of the epidural space. With both approaches, medication will often spread over several spinal segments and cover both sides of the spinal canal. With a transforaminal cervical epidural injection, often referred to as a ‘nerve block’, the needle is placed alongside the nerve as it exits the spine and medication is placed into the ‘nerve sleeve’. The medication then travels up the sleeve and into the epidural space from the side. This allows for a more concentrated delivery into one affected area (usually one segment and one side). Transforaminal epidural injection can also be modified slightly to allow for more specific coverage of a single nerve and can provide diagnostic benefit, in addition to improved pain and function.
All three procedures are performed on an outpatient basis, and you can usually return to your pre-injection level of activities the following day. Some patients request mild sedation for the procedure, but many patients undergo the injection using only local anesthetic at the skin.
After your epidural injection treatment, you will notice immediate pain relief due to the local anesthetic that is injected. This will wear off in a few hours, and pain may return briefly. The medication will take effect within a few days, soothing inflammation so that you can enjoy long-lasting pain relief. The results from your epidural injection can last between several weeks and several months. The exact duration of these results will vary, so we will help you determine the kind of results that you can expect during your initial visit.
Video Spotlight
Blog
Surgery-Free Solutions
Expert Tips for Pain Management
Testimonials
Words From Our Patients
The treatment was very good and the doctor Faraz Ahmed was very kind to the patient and explained clearly the procedure of knee bilateral ha & treatment And we were advised to do physiotherapy. We are very much satisfied. We would recommend this alleviate pain clinic. Thank you
Got treatment of Treatment and HA for right knee arthritis a month ago and finding good relief from pain. Was treated by Dr Swagtesh Bastia who explained very well about the injections and the treatment was painless. The front desk staff were very kind and very helpful and physiotherapy was also done expertly, overall good experience
Alleviate Pain Management clinic has been a godsend for my mom's knee pain. She has been treated by Dr. Wiquar Ahmed. The attentive staff provided personalised care, and after her treatment, she's feeling remarkably better. Thank you for giving my mom the relief she deserves!
The clinic is super clean with a great OT and most importantly all the staff here are very helpful and considerate. My gratitude to Dr Roshan, the nurses, and support staff - they were always available to assist with any issues post procedure and they even made an extra effort to make a home visit for a follow up check-up. This team here is the perfect example of healing and care with a human touch. Thank you!!!!!
My wife had knee pain I have visited alleviate pain and consulted doc santhoshi now she is able to walk pain free and can do her daily activity than before.the physiotherapist here Dr akhila also helped her with few exercises and the staff here Abdul explained all the procedures well . Thank you PPL can visit here for pain relief