Introduction
Pain can be a deceptive messenger. Often, the location of pain doesn’t necessarily indicate its true source. The human musculoskeletal system is a complex interplay of muscles, joints, nerves, ligaments, tendons, and blood vessels, and each of these components can be both the origin of pain and a source of referred pain, radiating discomfort to other parts of the body. Recent research has delved into understanding the structures behind referred symptoms and the intriguing mechanisms of pain referral patterns within the body.
Demystifying Dermatomes
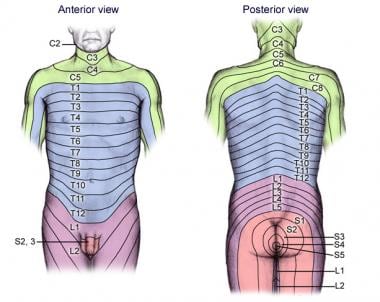
Dermatomes of the trunk and back
A dermatome is a specific region of the skin that receives sensory input from spinal nerves. When symptoms such as pain, numbness, or tingling follow a dermatomal pattern, it may suggest an issue related to the nerve root originating from the spine. Dermatomes are invaluable for pinpointing neurological levels, particularly in conditions like radiculopathy, characterized by pain, weakness, numbness, or muscle control difficulties. In cases of spinal nerve compression, symptoms may manifest within the corresponding dermatomal area in addition to weakness and reduced deep tendon reflexes.
Lumbar Facet Joints: A Common Pain Generator
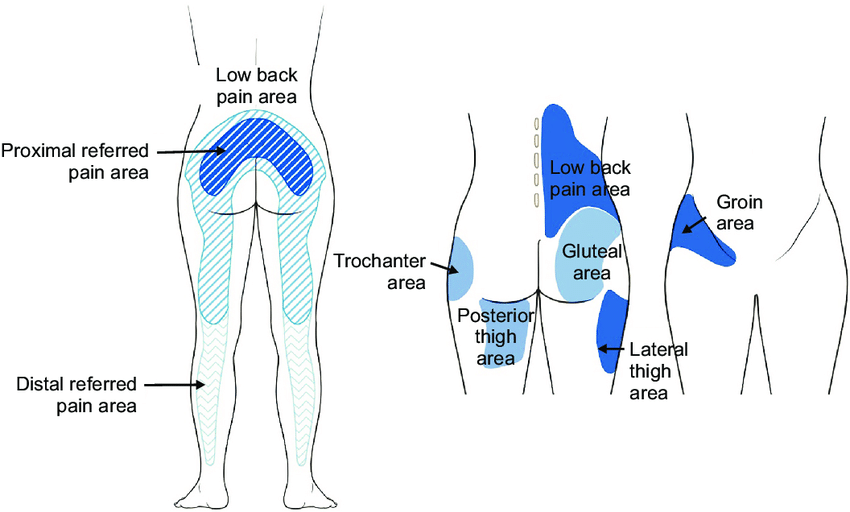
illustration of distribution pattern related to facet joint pain
Facet joints, the small joints found at each spinal segment, serve the dual purpose of providing stability and enabling motion. These joints can become sources of pain due to factors like arthritis, back injuries, or mechanical stress. Mechanical issues within the spine are commonplace, often stemming from everyday wear and tear or injuries that result in sensations like a “catch” or “crick”. Importantly, facet joint pain frequently refers pain distally, meaning away from the source. In the thoracolumbar region, where the thoracic and lumbar facets converge, a unique transitional zone exists. The orientation of these joints differs—lumbar facets allow for backward bending and toe touch, whereas thoracic facets enable side-to-side and torso rotation. Mechanical dysfunctions at this transitional point can mimic Sacroiliac joint pain, a condition known as Maignes syndrome. Moreover, facet tropism, wherein one side of the facet is oriented in the sagittal plane (flexion/extension) and the other in the coronal plane (side-to-side), is relatively common at this level, further complicating the clinical picture.
The Enigma of Sacroiliac Joint Dysfunction
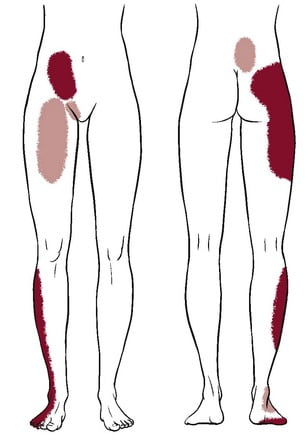
Sacroiliac joint pain radiation pattern
Sacroiliac joint dysfunction can trigger both localized and referred pain. The diagnostic tool known as the Fortin finger test involves the patient pinpointing the PSIS (posterior superior iliac spine) as the source of pain. The PSIS is located on the posterior aspect of the SI joint. Analyzing pain diagrams of 50 patients who underwent fluoroscopy-guided SI joint injections, Slipman CW et al identified common referral patterns from the SI joint:
- 94% experienced buttock pain
- 72% reported lower lumbar pain
- 14% described groin pain
- 50% felt pain in the lower extremities
- 28% experienced pain extending below the knee
These findings reveal the multifaceted nature of sacroiliac joint dysfunction and its diverse range of symptoms.
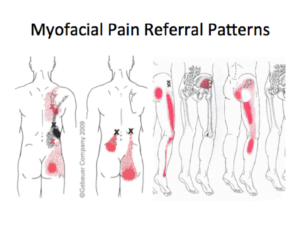
Unmasking the Myofascial Pain Puzzle
Muscles are another potential source of both local and distal referred pain. Myofascial pain often masquerades as facet or discogenic pain and can be misdiagnosed. In the lower extremities, muscles like the piriformis and gluteal muscles are known to mimic the symptoms of sciatica. Fortunately, myofascial pain can be effectively managed through techniques such as myofascial release and dry needling.
Hence it is essential to develop a deeper understanding the pain referral patterns of the sacroiliac joint, facet joints, and myofascial system to arrive at an accurate diagnosis. This helps in formulating an effective treatment plan to offer relief to patients suffering from musculoskeletal pain.
References
images taken from https:// www.pt360atl.com/