Introduction
The human knee is a remarkable joint, known for its intricate structure and vital role in our mobility. It’s composed of various components, including bones, ligaments, tendons, and cartilage, all working in harmony to facilitate smooth movement. However, the complexity of this joint also makes it susceptible to a wide range of injuries and conditions, including pain on the outside of the knee. This discomfort can be attributed to several factors, with some of the most common culprits being iliotibial band syndrome, lateral collateral ligament pathology, lateral meniscus tear, rheumatoid arthritis, osteoarthritis, and common peroneal neuralgia. In this comprehensive blog, we will delve into each of these causes, exploring their symptoms, diagnostic procedures, and treatment options.
Understanding the Anatomy of the Outer Knee
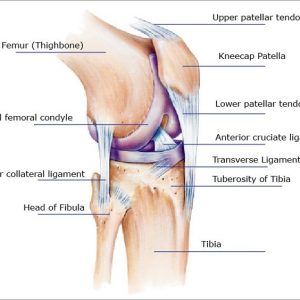
To comprehend the possible causes of outer knee pain, it is essential to first understand the intricate anatomy of the knee joint. The knee is one of the body’s largest and most complex joints, composed of the femur (thigh bone), tibia (shin bone), patella (kneecap), and a network of ligaments, tendons, and cartilage. The outer knee, in particular, is home to several structures that can become sources of discomfort.
The Iliotibial Band (ITB)
The iliotibial band is a thick band of fibrous tissue that runs along the outside of the thigh, from the hip to just below the knee. The ITB plays a crucial role in stabilizing the knee joint during movements. Overuse, friction, or inflammation of the ITB can lead to iliotibial band syndrome, a common cause of outer knee pain.
Lateral Collateral Ligament (LCL)
The lateral collateral ligament is one of the four major ligaments in the knee, providing stability to the joint by connecting the femur to the fibula. Injuries or damage to the LCL can result in lateral collateral ligament pathology, leading to pain and instability on the outer side of the knee.
Lateral Meniscus
The lateral meniscus is a C-shaped cartilage structure that acts as a cushion between the femur and tibia. Tears or degeneration of the lateral meniscus can cause pain, swelling, and discomfort, particularly on the outer aspect of the knee.
Rheumatoid Arthritis and Osteoarthritis
Rheumatoid arthritis (RA) and osteoarthritis(OA) are both degenerative joint conditions that can affect the knee. While RA is an autoimmune disease causing inflammation and cartilage damage, OA is a wear-and-tear condition that leads to the gradual deterioration of the knee joint. Both can cause outer knee pain and mobility issues.
Common Peroneal Neuralgia
Common peroneal neuralgia is a condition characterized by damage or irritation of the common peroneal nerve, which runs down the outer part of the knee. This condition can result in pain and weakness along the outer knee, lower leg, and ankle.
iliotibial Band Syndrome (ITBS)
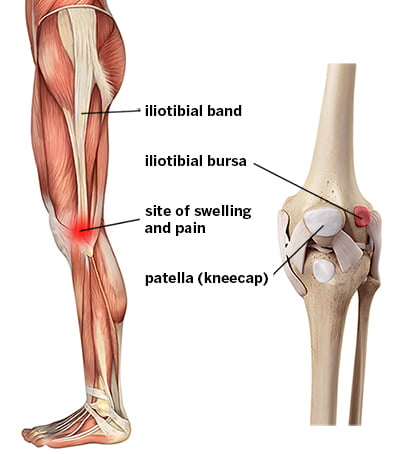
Iliotibial Band Syndrome, commonly referred to as ITBS, is a prevalent cause of outer knee pain among athletes and active individuals. The iliotibial band (ITB) is a thick band of connective tissue that runs along the outer side of the thigh, from the hip to the shin. When this band becomes tight or irritated, it can lead to pain on the outside of the knee.
Symptoms
- Pain or aching on the outer side of the knee.
- Pain can worsen with repetitive activities, such as running or cycling.
- Swelling and tenderness on the outer knee.
- A sensation of the ITB snapping over the femoral condyle.
Diagnosis
Diagnosing ITBS typically involves a physical examination and evaluation of the patient’s medical history. The doctor may perform a test known as the Ober test, which assesses the flexibility and tightness of the ITB. In some cases, imaging studies like MRI or ultrasound may be ordered to rule out other conditions.
Treatment
- Rest : Reducing or modifying activities that exacerbate the condition.
- Ice : Applying ice to the affected area can help reduce inflammation.
- Physical Therapy : Stretching and strengthening exercises may be recommended to improve flexibility and balance.
- Anti-inflammatory Medications : Over-the-counter or prescription medications may be used to alleviate pain and inflammation.
- Corticosteroid Injections : In severe cases, a corticosteroid injection may be considered.
- Activity Modification : Adjusting training techniques and using proper footwear can prevent recurrence.
PRP and Prolotherapy for ITBS
Platelet-Rich Plasma (PRP) and Prolotherapy have shown promise as treatment options for ITBS. PRP involves the injection of concentrated platelets from the patient’s blood into the affected area. These platelets contain growth factors that promote tissue healing. Prolotherapy, on the other hand, involves the injection of an irritant solution to stimulate the body’s natural healing response.
Several studies have explored the effectiveness of PRP and Prolotherapy for ITBS. A study published in the American Journal of Sports Medicine in 2018 found that PRP injections led to significant improvements in pain and function in individuals with ITBS. Another study in the Journal of Prolotherapy in 2019 demonstrated the potential of Prolotherapy in reducing pain and promoting tissue repair in ITBS patients. These minimally invasive treatments may offer relief for those suffering from ITBS.
Lateral Collateral Ligament Pathology
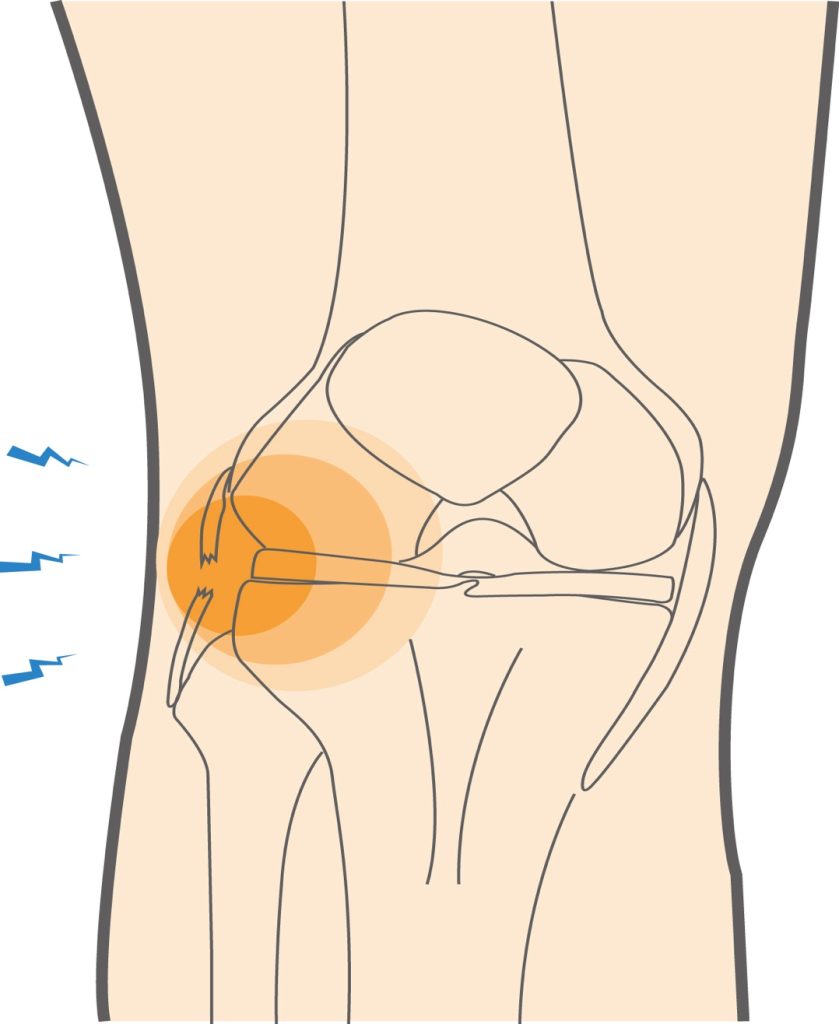
The lateral collateral ligament (LCL) is an important structure on the outer side of the knee that helps stabilize the joint. LCL injuries, though less common than anterior cruciate ligament (ACL) injuries, can result in lateral knee pain.
Symptoms
- Pain and tenderness on the outer aspect of the knee.
- Swelling and bruising.
- Instability of the knee joint.
- Difficulty bearing weight on the affected leg.
Diagnosis
To diagnose LCL pathology, a physical examination and a detailed patient history are essential. X-rays and MRI scans may be performed to assess the extent of the injury.
Treatment
- Rest : Avoiding activities that stress the knee.
- Immobilization : In some cases, a brace or cast may be required to stabilize the knee.
- Physical Therapy : Rehabilitation exercises can help strengthen the knee and improve range of motion.
- Surgical Intervention : Severe LCL injuries may necessitate surgical repair.
PRP and Prolotherapy for LCL Pathology
The application of PRP and Prolotherapy in LCL pathology is still an emerging field. However, preliminary research suggests their potential benefits. A study published in the “Journal of Orthopaedic Surgery and Research” in 2020 explored the use of PRP in the treatment of LCL injuries. The results indicated that PRP injections can enhance the healing process, reduce pain, and improve knee stability. Prolotherapy, too, has shown promise in promoting ligament repair, as discussed in a review published in the “American Journal of Physical Medicine & Rehabilitation” in 2017.
Lateral Meniscus Tear
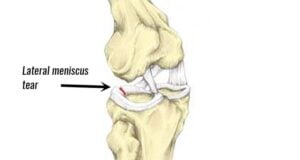
The meniscus is a C-shaped cartilage in the knee that acts as a cushion and helps with joint stability. Tears in the lateral meniscus can lead to outer knee pain.
Symptoms
- Pain on the outer side of the knee, particularly when twisting or pivoting.
- Swelling and stiffness in the joint.
- A feeling of the knee giving way.
Diagnosis
A thorough evaluation by a medical professional is crucial to diagnose a lateral meniscus tear. MRI scans are commonly used to assess the extent and location of the tear.
Treatment
- Rest : Reducing activity to prevent further damage.
- Physical Therapy : Strengthening exercises can help improve joint stability.
- Arthroscopic Surgery : Surgical repair may be necessary for severe tears.
PRP and Prolotherapy for Lateral Meniscus Tears
The use of PRP and Prolotherapy for lateral meniscus tears is an active area of research. A study in the “Journal of Knee Surgery” in 2019 suggested that PRP injections can improve pain and function in patients with lateral meniscus tears. Prolotherapy has also demonstrated positive outcomes in encouraging meniscal repair, according to research published in the “Journal of Sports Science & Medicine” in 2020.
Rheumatoid Arthritis
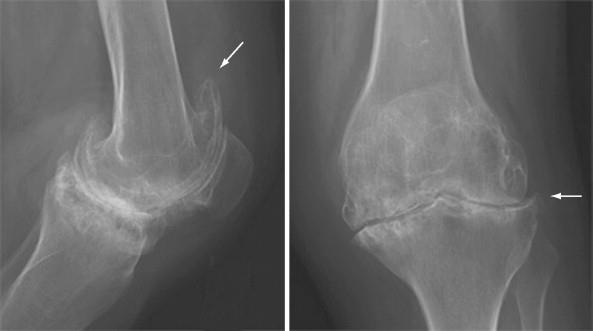
RA with secondary OA and severe cartilage loss. Radiographs of the knee show severe uniform loss of the cartilage space. The symmetry of medical and lateral compartment narrowing suggests an underlying inflammatory condition. The changes of OA with osteophytes (arrows) and subchondral sclerosis are noted. Soft tissue swelling and a suprapatellar knee effusion are also present.
Rheumatoid arthritis (RA) is a systemic autoimmune disease that can affect various joints in the body, including the knee. In the knee, RA can lead to outer knee pain due to inflammation and damage to the joint.
Symptoms
- Pain, swelling, and warmth in the knee.
- Morning stiffness that lasts for more than 30 minutes.
- Reduced range of motion.
Diagnosis
Diagnosing RA involves blood tests to check for specific antibodies and imaging studies to assess joint damage. A thorough examination of the affected joint is also essential.
Treatment
- Medications : Disease-modifying antirheumatic drugs (DMARDs) and biologics are often prescribed to manage RA.
- Physical Therapy : Exercise and rehabilitation can help maintain joint function.
- In some cases, surgical procedures like joint replacement may be necessary.
Osteoarthritis
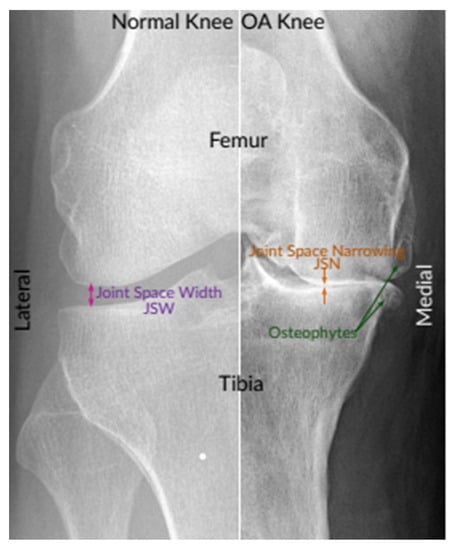
An instance of X-ray images of the normal knee and severe OA knee. On the left is a normal knee, and on the right is an OA knee. This image shows joint compartments, as well as joint space narrowing (JSN) and osteophytes
Osteoarthritis (OA) is the most common form of arthritis, often referred to as “wear and tear” arthritis. It can affect any joint in the body, including the knee.
Symptoms
- Pain on the outer side of the knee, which may worsen with activity.
- Stiffness and limited range of motion.
- Joint crepitus (cracking or grinding sensation).
- Bony growths (bone spurs) around the joint.
Diagnosis
A combination of clinical assessment, imaging studies (X-rays, MRI), and sometimes joint fluid analysis is used to diagnose OA.
Treatment
- Medications : Non-steroidal anti-inflammatory drugs (NSAIDs) can help manage pain and inflammation.
- Physical Therapy : Exercise programs can improve joint function and reduce pain.
- Injections : Corticosteroid or hyaluronic acid injections may be recommended.
- Surgical Options : In advanced cases, knee joint replacement surgery may be considered.
PRP and Prolotherapy for RA and OA
PRP and Prolotherapy have been studied as potential treatments for both RA and OA. In a review published in “Rheumatology International” in 2021, PRP therapy was found to provide pain relief and improve knee function in RA patients. Prolotherapy, as discussed in a study in the “Journal of Prolotherapy” in 2018, showed promise in stimulating tissue repair and reducing pain in OA patients.
While these therapies offer potential benefits for RA and OA, they are often used as complementary treatments alongside conventional approaches. Consultation with a rheumatologist or orthopedic specialist is crucial for creating a personalized treatment plan.
Common Peroneal Neuralgia
Common peroneal nerve entrapment, also known as common peroneal neuralgia, can lead to pain on the outer aspect of the knee. The common peroneal nerve runs close to the surface on the outer part of the knee, making it susceptible to injury or entrapment.
Symptoms
- Pain, tingling, or numbness on the outer side of the knee and upper shin.
- Weakness in the muscles of the lower leg and foot.
- Difficulty lifting the foot (foot drop).
Diagnosis
Diagnosis typically involves a detailed neurological examination and, in some cases, nerve conduction studies or electromyography (EMG) to assess nerve function.
Treatment
- Rest : Reducing activities that exacerbate the condition.
- Physical Therapy : Exercises can help strengthen the affected muscles and improve foot dorsiflexion.
- Orthotic Devices : Braces or splints may be used to support the foot and ankle.
- Surgical Decompression : In severe cases, surgical release of the entrapped nerve may be necessary.
The Role of PRP and Prolotherapy in Knee Pain Management
Platelet-Rich Plasma (PRP) and Prolotherapy are gaining attention in the field of orthopedics for their regenerative and pain-relief properties. The primary mechanism behind these treatments lies in their ability to stimulate the body’s natural healing processes. PRP involves the injection of a concentrated solution of platelets, growth factors, and other bioactive substances derived from the patient’s blood. Prolotherapy, on the other hand, entails the injection of a solution that causes a controlled, localized irritation, which promotes tissue repair.
While the specific effects of PRP and Prolotherapy can vary based on the condition being treated and the individual patient, potential benefits include:
- Reduced Pain : Both PRP and Prolotherapy have been shown to reduce pain in various knee conditions, allowing patients to regain mobility and improve their quality of life.
- Improved Function : These therapies can enhance joint function and stability, helping individuals perform daily activities and engage in physical exercise with greater ease.
- Tissue Repair : PRP and Prolotherapy stimulate the body’s natural healing processes, potentially promoting tissue repair and regeneration in damaged or degenerated areas.
- Minimally Invasive : These treatments are typically minimally invasive, with a low risk of adverse effects or complications, making them suitable options for many patients
Conclusion
Pain on the outside of the knee can result from a variety of underlying causes, ranging from overuse injuries and structural issues to systemic conditions like arthritis. We at Alleviate Pain Clinic believe in a thorough clinical and radiological evaluation leading to an accurate diagnosis and appropriate treatment plan for managing and alleviating the discomfort associated with outer knee pain. If you or someone you know experiences persistent knee pain, it’s essential to seek medical advice from a qualified healthcare professional. Early intervention and a tailored treatment plan can often lead to successful outcomes, allowing individuals to regain mobility and lead a pain-free life.
As with any medical condition, the information provided in this articleis for general informational purposes and should not be used as a substitute for professional medical advice. Always consult a healthcare provider for a comprehensive evaluation and personalized treatment recommendation